Last month a pre-print was published that showed COVID-19 antibodies in South Africa had reached remarkably high levels. It was ignored by most of the media, but given the concern over the South Africa variant being “more transmissible” and “evading vaccine immunity” it shouldn’t have been as it gives an indication of what we might expect from the variant.
Extrapolating from antibody testing on blood donors, the researchers found antibody levels of 63% in Eastern Cape province (EC), 46% in Free State (FS), 52% in KwaZulu Natal (ZN) and 32% in Northern Cape (NC). These figures were between 15 and 22 times higher than the percentage of the population that had tested positive for the virus to date.
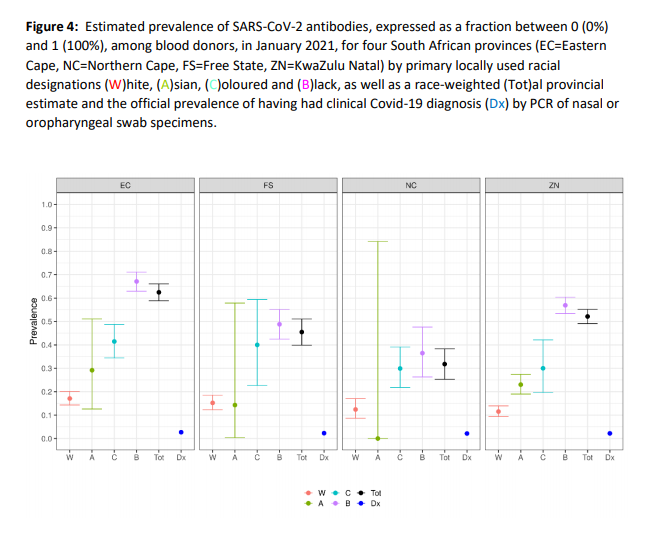
Major differences were found between races. Seroprevalence among black donors was consistently several times higher than among white donors, which the authors put down primarily to the difficulty in social distancing among the lower income black communities. As black people form the majority in the country, this meant seroprevalence among black people in each province was slightly higher than the overall seroprevalence (see graph above). Seroprevalence among white people was between 10% and 18% – figures notably similar to those found in European countries pre-vaccination. The authors attributed that to the effectiveness of social distancing and lockdowns, which they considered white people in general to be in a better socio-economic position to observe.
Be that as it may, it is notable that, notwithstanding the lack of vaccinations, the “more transmissible” variant and, as the researchers acknowledge, little effective social distancing, cases and deaths peaked and sharply declined from mid-January. As of March 9th, the Covid death toll in South Africa stands at 858 per million, less than half the UK’s 1,842 per million. This may under-count the true death toll, though there is no evidence of a great deal more deaths in the country that have gone unreported.
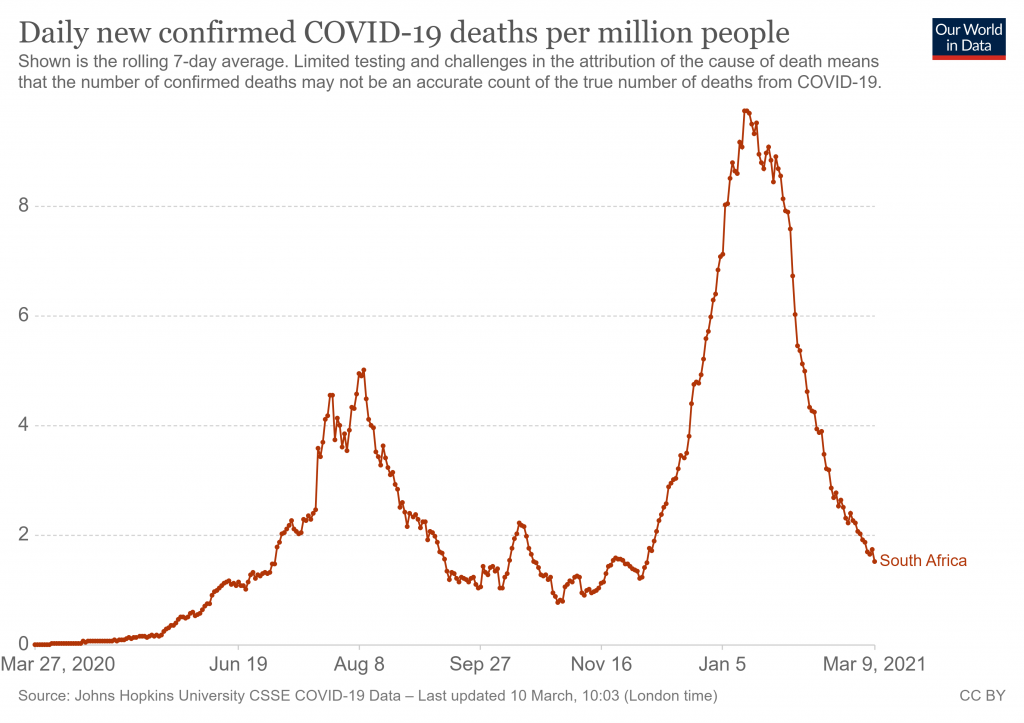
What caused this decline? With antibody prevalence as high as 63% in some areas (let alone other forms of immune resistance, such as T cells) collective/herd immunity has to be a prime suspect. Another factor may be the fact that January is the middle of summer in the southern hemisphere (though, interestingly, that didn’t prevent the spike in the first place).
Worth noting, though, that there is nothing unusual about a COVID-19 epidemic going into spontaneous decline, even with antibody prevalence much lower than in South Africa. Places with few restrictions such as Sweden, Florida and South Dakota have also seen spikes fall almost as quickly as they have risen, and at much lower antibody levels – and in the middle of winter, too. Spontaneous decline is in fact the norm for a COVID-19 outbreak, not the exception, as we saw when new daily infections in England peaked ahead of the national lockdown on all three occasions. Happily, the South Africa variant does not appear to alter this basic behaviour of the virus.
Today, March 11th, we mark the anniversary of the WHO declaring a pandemic and the beginning of the steep slide into the eternal lockdown in which we now find ourselves. A good moment, then, to reflect on whether it has all been worthwhile and what it has achieved. If South Africa is any indication, the tragic answer is: nothing at all.













To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.
Even after the first “wave”, 48% of blood donors in a Cape Town township was found to have antibodies to SARS-Cov 2. Our second “wave” during summer dropped off naturally – second lockdown consisted of a curfew, no nightclubs, compulsory masking (in and out doors) and a beach ban(!). Otherwise business as usual.
Many hospitalized patients died through neglect – no fluids/food, oxygen running out etc. Hospital beds were added, but there was no staff to man them. I don’t know how our overworked medical staff will cope with the mental strain of working under such monumental administrative failures.
However the economy trashed by the ANC. Wine growers not allowed to produce wine. This is just the tip of the iceberg.People impoverished. I weep for the country of my birth.
http://www.the-buyer.net/opinion/bruce-jack-covid-19-devastating-impact-on-south-africa/
“I weep for the country of my birth“
… as I do for the much more privileged country of mine!
“no nightclubs, compulsory masking (in and out doors) and a beach ban(!). Otherwise business as usual”.
The masks are the problem and wearing them in and out of doors is a major health hazard.
And there are flights in and out of Scotland right now that connect on to South Africa but ‘The English’ are not permitted to travel into Scotland.
That, and the recent contempt shown for its national assembly, assembly committees, by its assembly leader, tells you all you need to know about the state of Scotland today.
It seem to have taken a long time for some people to have got the message. It’s been plain for many many months that lockdowns don’t work and that they cost lives. The government will never hear this message because it doesn’t fit in with the sinister vaccine agenda.
I respect your view re. vaccines but I do not believe there is any sinister agenda. I do believe that Boris and his ministers’ cabal has dug a hole for itself and now won’t consider anything else but lockdown. They have never had a strategy and stuck to it. At the outset it was herd immunity, eat out to help out and back to work. Then it was lockdown and vaccinate.
Nothing about the incompetence/panic theory really stacks up. With rare exceptions most countries have adopted the same crazy approach to Covid-19, while they all parrot the same drivel, straight from the copybooks of Klaus Schwab and the great depopulator himself, Bill Gates. If he had wanted to, Boris could have got out of this bind scot-free last summer, when cases dropped away to near nothing, he could have triumphantly claimed lockdown success and got us quickly back to normal. But no, all we got was more talk of vaccines being the only way out, while a few meaningless restrictions were temporarily relaxed. At the same time measures like the unscientific mask mandates were being further tightened up. Boris then championed the costly and exponential ramping up of the utterly unreliable unfit for purpose PCR tests. Clearly this was a major effort to conjure up hundreds of thousands of Covid cases, out of healthy people. Everything about the UK government’s handling of Covid points to a firm intention to coerce a frightened public into rashly “volunteering” for the hardly tested experimental Covid “vaccines”that aren’t vaccines. These highly “sinister” offerings are already causing the the bodies to stack up, while the longer… Read more »
I think that this item potentially highlights the critical futile stupidity of lockdown.
Of course, it doesn’t constitute ‘proof’, but there is a high probability that the critical differences between racial groups illustrates the fact that lockdown simply inhibits the natural processes of population immunity.
As pointed out in the article, it is highly likely that the white population has been able to isolate itself more ‘effectively’ – with a detrimental overall outcome.
This would fit in with the wider evidence re. lockdowns, and the higher than expected surge in infections in this country, peaking in January.
I’m in SA now spending time in the Eastern and Western Capes. Aside from mask wearing (anywhere in seems but over nose and mouth) matters are normal.
Seems to me that people are generally slimmer and fitter than the unfit couch potatos in UK which is probably also a factor.
There were riots at Knysna in early Feb with the N2 blocked with burning tyres. The placards said tourists bring jobs.
SA has it’s problems but it seems to have handled covid much better than UK. The £ billions wasted in the UK could have been put to much better use here.
Careful with jumping to conclusions on data based on blood donors! There are specific factors here: blood donors are the group who tend to take more risks than common folks. They’re more likely to leave home, care less about their personal safety, so they’re more likely to get infected. They’re healthier too, which means that they’re less likely to develop serious symptoms if they catch coronavirus. Considering the above, the antibody prevalence in this specific group may be much higher than in general population. This was the case of Manaus, Brazil where authorities were convinced that the city has already achieved herd immunity because majority of blood donors had antibodies. This was mistake, the city went through another deadly wave shortly after.