On Lockdown Sceptics we have highlighted before the reasons that restrictions don’t have the expected effect of suppressing COVID-19. Partly it’s because lockdowns don’t prevent spread in hospitals, care homes and private homes, where much of the transmission happens, especially that which leads to serious disease. And partly it’s because people who are infectious and symptomatic fail to self-isolate, perhaps because they cannot, or cannot afford to, or because they think it’s just a cold.
It’s not because asymptomatic infection is a major driver of transmission. Despite this claim being much repeated, including by public health authorities, the evidence is that (as with other similar viruses) asymptomatic infection is barely infectious and contributes very little to the spread of the coronavirus.
We now have some clear data on how many people who develop COVID-19 symptoms actually follow through with self-isolation. A large nationally representative survey of 53,880 people published this week in the BMJ finds that less than a fifth (18%) of people who have COVID-19 symptoms take a test and less than half (43%) of those with symptoms (and who don’t test negative) fully self-isolate for 10 days without leaving home. Even at the height of the January surge, when hospitals were being stretched, only 52% of people with symptoms (and no negative test) fully self-isolated.
The survey asked the reasons for breaking the quarantine.
The most frequently reported reasons for not fully self-isolating were to go to the shops for groceries or to a pharmacy (21.5%), to go to work (15.8%), to go to the shops for things other than groceries or pharmacy goods (15.6%), because symptoms did not persist or were temporary (15.2%), to go out for a medical need other than COVID-19 (15.0%), to go for a walk or for some other exercise (14.8%), believing symptoms were only mild (14.5%), because symptoms got better (13.9%), thinking it was not necessary to stay at home (13.2%), being too bored (12.2%), to help or provide care for a vulnerable person (11.9%), to meet up with friends or family, or both (11.3%), and being too depressed or anxious (11.2%).
It also asked about reasons for not requesting a test.
The most common reasons for not requesting a test were thinking the symptoms were not due to COVID-19 (20.9%), symptoms had improved (16.9%), symptoms were only mild (16.3%), having no contact with anyone who had COVID-19 recently (13.0%), thinking that only self-isolation was needed (11.5%), not wanting to use a test that someone needed more (11.1%), not thinking you were eligible to get a test (11.0%), and being worried about how colleagues or employers would react if a test result was positive (10.0%).
This confirms there is no reason to believe in the evidence-free concept of widespread asymptomatic transmission to explain why lockdowns don’t work. With more than half of people who have symptoms not fully self-isolating, that’s plenty of opportunity for symptomatic transmission.
In terms of evidence that lockdowns don’t work, we now have a new study to add to our ever-growing list.
Christian Bjørnskov, a Professor of Economics at Aarhus University in Denmark, has this week published a study, “Did Lockdown Work? An Economist’s Cross-Country Comparison“, in the Oxford academic journal CESifo Economic Studies. The study explores “the association between the severity of lockdown policies in the first half of 2020 and mortality rates”. In a sophisticated analysis that draws on the Blavatnik Centre’s COVID-19 stringency index, Professor Bjørnskov addresses “policy endogeneity in two different ways” and takes “timing into account”, and concludes he can find “no clear association between lockdown policies and mortality development”.
This conclusion is confirmed by looking at how U.S. states have fared which eschewed lockdown orders or have recently lifted them.
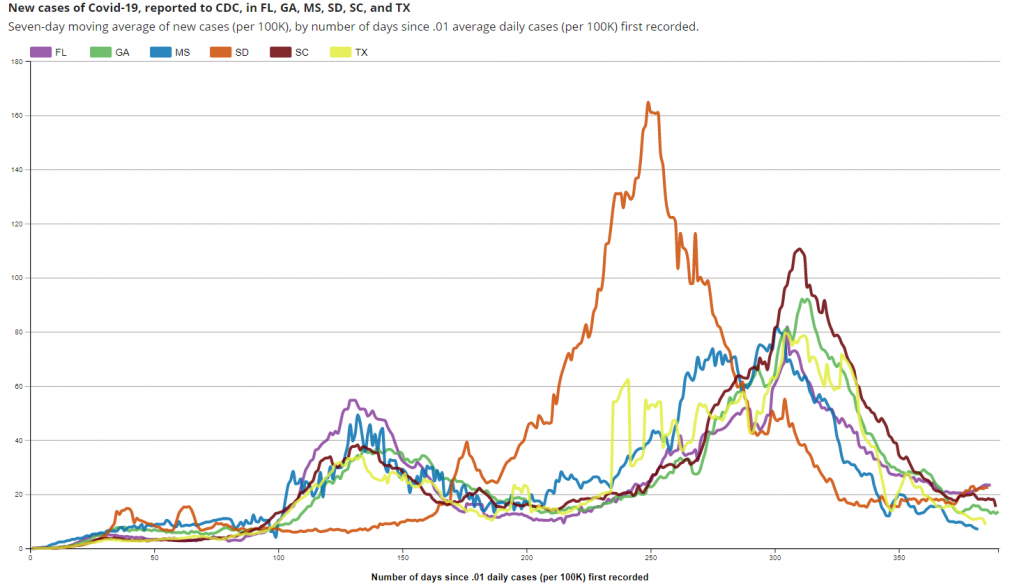
The graph below depicts the positive case curves for six states which currently have no restrictions at all, whether because they never had them (South Dakota), because they removed them after the first wave in the spring (Georgia and South Carolina) or the autumn (Florida), or because they removed them in the last few weeks (Mississippi and Texas). All have seen positive cases and deaths tumble with no sign (yet) of a spring resurgence. Contrary to all the epidemiological models, the absence of restrictions and masks has not resulted in mass hospitalisation and death amongst the population, regardless of when the restrictions were removed. All have followed similar trajectories to one another as well as to states which imposed far more restrictions.
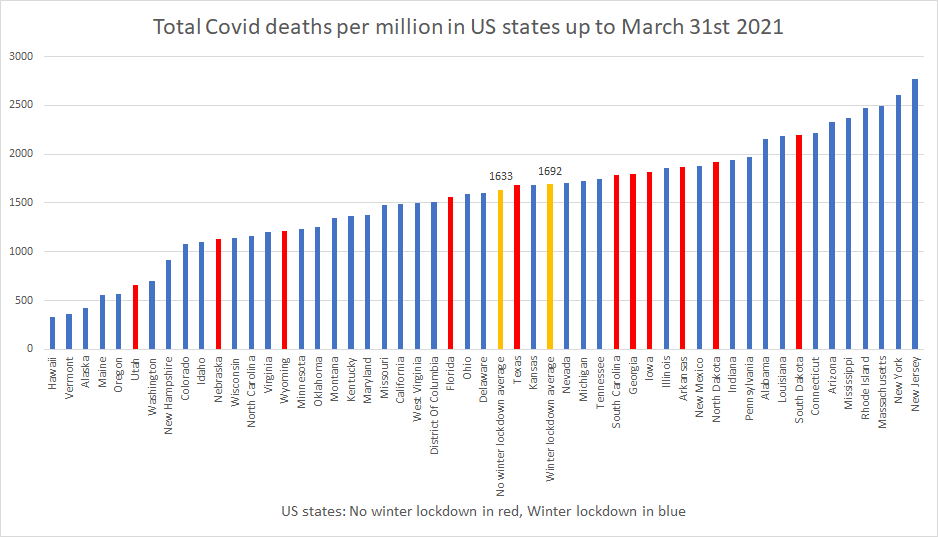
Below is a chart with the up-to-date Covid death tolls per million people for U.S. states. It shows that mortality remains lower on average in states which did not lock down (i.e., impose stay-at-home orders) during winter compared to those which did.
The evidence is clear: lockdowns don’t work, they aren’t necessary and they cause great harm.













To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.
What I can never understand is how people, despite being so unwilling to isolate when it is THEM being restricted are so happy to insist OTHERS stick to lockdown diktats. How low and foul a human being can you be to think that others should be restricted and you not? All the zealots try to tell me I am a villain, but I’m the one who stands for consistency, freedom for EVERYONE, I say one law for all (and not the state’s law any more, back to magna carta until we can write up something better than today’s totalitarianism). I support all who defy lockdown diktats, but I’m sickened by the thought of people who can be so warped as to want enforced upon others that which they do not accept done unto themselves.
A lot (most?) people will always act in what they consider to be their own self interest and human beings everywhere are masters of rationalising their actions.
The riddle of our being.
It’s a strange mentality. The people of the U.K. seem very happy for their government to brutalise the people of this country. Many in fact, are demanding the government is even harsher with longer tougher lockdowns and more penalties and more freedoms surrendered but strangely do not seem to think any of this applies to them as individuals. This is evidenced by the Sara Everard ‘vigil’ – the very same people who were more than happy for the government to ban public gatherings and for the police to stop and beat up anti lockdown protesters then could not understand why the police did the very same thing to them when they held a public gathering.
This is what I am struggling with in regard to the older, vaccinated population. They were screaming at young people to stay at home; I personally got shouted at in the street last summer for not “moving aside” as an elderly couple walked past me (me, an nhs doctor). Yet now they are vaccinated they’re out and about visiting friends and family – which I agree we should all be allowed to do. It’s the double standard though. The arrogance of expecting the young to sacrifice their lives to save the old and the old, the minute they’re no longer as personally concerned, throwing caution to the wind. Despite the supposed fact that they can still spread the disease to others.
Typical of that generation, they have always been selfish. Like you say it is wrong on so many levels the young are been sacrificed so that the old (most of whom have far exceeded a reasonable life expectancy) can eek out a few more years at the end of long, prosperous and even more importantly free lives.
The BBC, perhaps surprisingly, gave a partial report on the BMJ article yesterday.
One of the things they highlighted was that only half of people know what the main symptoms of Covid are.
This is patently false after a year of relentless information/propaganda about what Covid symptoms are (granted ever increasing in number).
What those people really meant was
‘ I probably had the Covid but I can’t afford to have ten days unpaid off work and neither can my partner so we just pretended not to know. Anyway we’re still here so no harm done’.
“Main symptoms of COVID”. Do you mean the main symptoms now, the symptoms a month ago, or in January, or in December? Because the list of symptoms changes all the time, and now includes just about every symptom of mild illness.
I thought “what are the symptoms of COVID” was an easy question. Turns out it’s hard. If we get this question right, can we go to the pub in a normal way?
No? Thought not…
It’s not about ‘what I meant’, I’m just the messenger.
Since we’re on holiday here’s something cheerful spotted in a local coffee shop window.
Apologies, I never meant my comment as a dig at you: more of a sarcastic take on the ridiculous, ever-changing scope of what counts as a COVID ‘symptom’. Sorry if my choice of language didn’t make that clear.
Love the pic!
Wasn’t taken as such st27, looks like the sun is finally arriving today, let’s all get down to the park and mingle !
Good point – the ‘cleverness’ of government in creating a hysterically exaggerated catastrophe was always going to backfire – whether it was the confusion related to numbers or the endless list of symptoms.
A message to all Covid cretins everywhere:
LOCKDOWNS DON’T BLOODY WORK BECAUSE HOWEVER LONG YOU HIDE AWAY, THE SODDING VIRUS IS STILL OUT THERE.
got that, you imbeciles?
No, of course you haven’t.
You could also add:-
If you are fit and healthy you have a very good chance, at least 90% of a full recovery so what’s there to worry about!? Your 99 year old Gran Might not be so lucky but she should have had the vaccine by now and anyway, let’s face it because she is 99 she is going to die soon anyway, Covid or no Covid.
That latter view was originally aired by a medic/journo (?) just about 12 months ago. At first it was given a bit of attention before the press decided that the idea was intolerable inhumàn so it and the messenger were buried in a slurry pit of hate.
… and the vaccine may have been what pushed her over the edge.
“In terms of evidence that lockdowns don’t work, we now have a new study to add to our ever-growing list.”
I’d live through 10 more lockdowns as long as I never had to hear the expression “in terms of”.
(Well, I wouldn’t, but perhaps you know what I mean)
“people who are infectious and symptomatic fail to self-isolate, perhaps because they cannot, or cannot afford to, or because they think it’s just a cold”. There’s a very good chance that it is just a cold.
The survey is junk. Those who never got a test because they didn’t think it was Covid for example, how do we even know it was Covid? Maybe they were right. How would they ever know?
It’s just assumptions based on ridiculous PCR tests anyway.
These responses are not surprising and any good psychologist should have be able to predict them. It is a pity they didn’t have any psychologists on SAGE who could have worked this out.
But of course they were too busy working out how to scare the compliant sh**less.
If I remember right, the basis evidence for the original mid-December NERVTAG paper which ‘proved’ that UK Variant (ZOMG! Run For The Hills!) is so much more infectious was an ‘unexpected’ (according the Model) sharp rise in ‘case’ numbers. (Coronanonsense is resulting a global shortage of scare-quotes – go long on them, you read it here first!).
There are more possible reasons for that rise, which the paper didn’t even consider, than I have room to list. But the most glaring one is the possibility that either lockdowns don’t work, or that people aren’t actually even following the rules.
But the conclusion, of course, was that UK Variant (ZOMG etc) ‘must be 70% more infectious’.
Mid December – when everyone is flooding the shops for Christmas shopping.
In January Local Live ‘(mirror group news) warned that the scary Kent mutant was now dominant throughout the County yet whenever I asked anybody during the next few weeks it had seemingly vanished.
Thanks Will for a brilliant report which is exactly on the spot. The disease is in many and most cases so mild that there is difficult for anyone affected to isolate for a sniffle. This, I think, is perhaps a difference with flu. In many flu cases the symptoms are harder with high fever and severe muscle pains. You are sick and stay in bed for the infectious period. This is the brutal paradox with influenza and might explain the higher R. So many mild cases running around infecting a few with a severe disease outcome. Perhaps better idea of isolating the risk groups from the beginning?
You also need an economic reason to stay home, full payment for sick leave. In Sweden at the beginning of pandemic the usual rule was no payment for first 2 days off sick than full payment for a week. This was quickly changed to full payment from the first day of sick leave and encouraging sick leave for trivial sniffle. They knew it could be abused and had a price to pay, which was low considering the slight reduction in Sweden’s GDP compared to UK’s world record
“the higher R”
‘R’ is simply another modelling fiction on the GI>GO trail.
Remember in the early days Wilko saying they would not be flexible over sick leave in case staff abused the system? That’s exactly the attitude here – even though we have lost eye-watering amounts of money with lockdowns, the idea of a small number of people taking the p*ss is just too intolerable, even if it is for the greater good. We have always had an appalling culture of ‘sickness presence’ in workplaces, with people clearly unfit to work walking around spreading disease, scared to take a sick day even if they were allowed paid leave. And instead of just addressing that we lose our minds expecting perfectly healthy ‘exposed’ people to self-isolate repeatedly at the drop of a hat on pain of a £1,000 fine. No doubt the government response to this will be to bring in higher fines, and more intrusive surveillance. Don’t forget in Australia they have been tagging people. And let’s not forget Labour and Libdems are absolutely on board with that, whatever they say about opposing the coronavirus act and vaccine passports.
And now 50% of adults have had the gene therapy and will show no symptoms, this has made it more likely they’ll pass it on and less likely they’ll stay at home… I want this on a t-shirt: The chance of death is 100% – now can we all start living.
It’s such a dangerous disease that less than half of those with symptoms isolate, they just go about business as usual
All those naughty infectious people going to the supermarket and not a single one shut due to a covid outbreak on the entire 12 months. Especially interesting considering there were no masks in the first lockdown, no hand sanitizer (you couldn’t get supplies) and it was quickly apparent (in a smaller supermarket like where I work) that social distancing was impractical for the staff. This is why pretty much everyone where I work thinks it’s all bollocks.
I still use the same small Tesco and large Co Op as before and the staff are still virtually the same, none has replaced colleagues who have fallen for the Covid.
They were only obliged to start wearing masks to placate the shoppers when they were forced to.
‘If we got to wear masks how come the staff don’t?’
“We now have some clear data”
No we don’t. I’m not knocking the attempt, but self-reporting survey data is, by its nature, fraught with problems. On top of that, you have the miasma of perceptions about Covid, the falsification of basic data, and the distorted reactions created by the Fear agenda.
It is probable that a clear and realistic focus on the known measures such as self isolation when symptomatic would have been more successful if it had not been contaminated with the confusion and exaggeration introduced by pole-climbing seekers of significance in the public health field.
Throughout this madness I have been determined to carry on as normally as I’m able to. I haven’t been sanitising or washing my hands more than usual, I haven’t worn a face covering in shops etc. I also vowed I would never take a COVID test. However tomorrow I am booked in for such a test much to my annoyance and disappointment. The reason ? apparently I cannot have an important medical procedure in hospital without a negative test. I can’t help feeling angry with myself for betraying the cause.
So still blame the people, then.
A year ago our Imperial Government locked us down with no strategies for delivering food or medicine to those at home with Covid. If you felt ill you still had to rush to the crowded shops. I had Covid then and had to go onto street mail to appeal to strangers to get pain-killers. Many who were presymptomatic and infectious must have gone to shops and pharmacies to help others who were sick in their houses. It is likely that the start of lockdown itself drove infection rates up in those early days.
In those early days ill people like yourself were urged to stay home and only trouble the NHS if their symptoms became worse.
This meant that by the time they got to hospital they had already been unwell for several days and were denied the benefit of early medical intervention.
Hence higher hospital mortality at the start.
People with symptoms not self-isolating doesn’t surprise me at all – long before Covid19 showed its face I recall people turning up to work armed with boxes of tissues, lemsips and nasal sprays to ease their cold and flu-like symptoms – spreading it all around the office – soldiering-on regardless just to impress the boss and show how dedicated they were to their jobs. If I ever tried to get a day off work with a bad cold I would be regarded as a skiver and repremanded.
Yes we had a manager who would come into work coughing and spluttering over everyone. Then he dragged in everyone who had more than one sick day in three years and gave us a verbal warning.
I wonder how he’s doing now.