Last week I wrote that U.S. states which locked down over the winter had a higher Covid death toll on average than those which did not.
Some people argued that I should have only looked at deaths over the winter rather than in total for it to be a fair comparison. I disagree. That would mean places which had a high death toll in spring would look better just because they had already been hit hard, lost a lot of people, and built up some immunity. Also, in lockdown theory, lockdowns only defer deaths, they don’t prevent them, so any state which didn’t lock down in winter should have suffered then any deaths deferred by earlier measures. Thus the fairest comparison for understanding whether lockdowns are necessary to prevent a catastrophic death toll – the central claim at stake – is the total number of deaths, not just those in one season.
Today I’m updating the figures. At the same time I’ve done a fresh review of the measures different states took (using these two handy websites which have collected them all together) to ensure I’m putting each state in the correct category.
Nineteen states issued an actual stay-at-home order this winter. While most of these (except for Oregon and New Mexico) were advisory, they all made clear that people should stay at home as much as possible and were accompanied by other severe restrictions such as business closures and bans on gatherings. A further 14 states, though not issuing a stay-at-home order, imposed similar strong restrictions that served the same basic purpose. These I’ve classified as the winter lockdown states (they include Washington, D.C.).
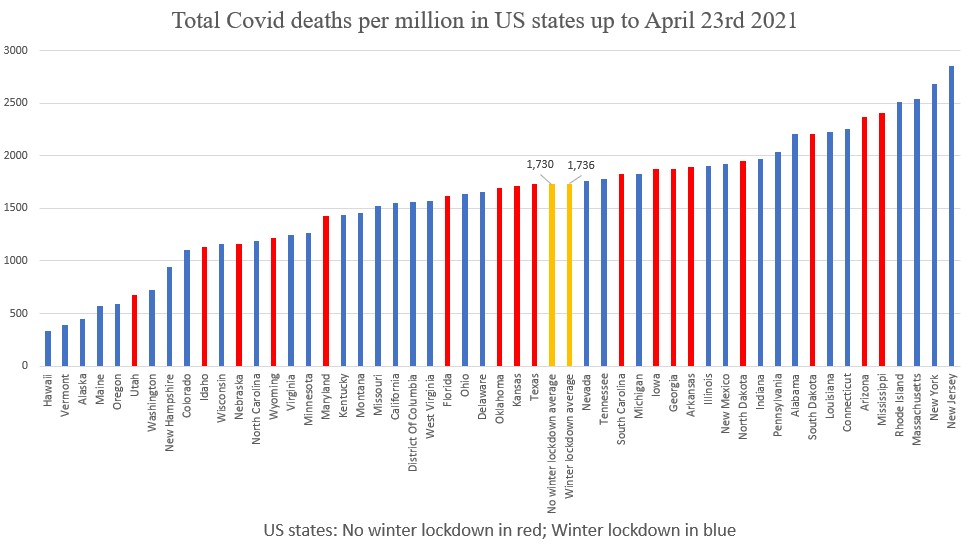
The other group of states imposed much lighter restrictions, such as business capacity limits (often around 50%) or gathering limits (such as 50) but did not issue a stay-at-home order, close businesses or ban private gatherings. There are 18 of these – the 11 I included last time, plus seven I’d overlooked, including Arizona and Mississippi. These two states in particular are up in the top six states states for Covid deaths per million so I was concerned this would shift the average for the no-lockdown states above the lockdown states. However, the no-lockdown states still come out lower (albeit with a smaller gap) – 1,730 vs 1,736. (Death and population data from Worldometer.)
As noted before, we shouldn’t get too hung up on the precise numbers here, which will be affected by various factors such as the population density and demographics of the state and the precise way the state counts Covid deaths. The important point is the big picture: the fact that in one big country with lots of different regions responding to an epidemic in different ways, there was no obvious relationship between interventions and outcomes. In particular, those which didn’t lock down did not suffer “hundreds of thousands” more deaths (or the population-size equivalent) than those which did, contrary to what all the mathematical models predicted. Their epidemics peaked and declined in the same way as lockdown states.
This point becomes even clearer when we focus in on the six states which kept restrictions to a minimum this winter – Florida, Georgia, South Dakota, South Carolina, Utah and Nebraska. These states had 1,629 Covid deaths per million on average, well below the 1,736 average of the lockdown states.
Some might want to quibble with which category some of the more middling states in terms of severity of winter restrictions should go in. Given how close the two groups are when it comes to deaths per million, I wouldn’t be surprised if a subtle shifting of criteria could put the no-lockdown states just ahead in terms of total deaths. (For example, you could argue about whether Maryland’s restrictions belong in the strong or light category.) But this wouldn’t change the big picture – that lockdowns are not preventing mass deaths from COVID-19, they are not holding back the flood. Rather, they are making no discernible difference to outcomes, despite their immense social and economic costs and the disruption they cause to people’s lives.
I have addressed before why, despite their intuitive appeal as a way of suppressing viral spread, lockdowns have no significant effect on controlling the coronavirus. The chief reason is because much of the spread, particularly that which leads to serious disease and death, occurs in hospitals and care homes. Forty per cent of Covid deaths in England and Wales in the spring were care home residents, while Public Health Scotland found that between a half and two thirds of serious infections in the winter were picked up in hospital. Between these and transmission in private homes (which is more likely to happen when people are forced to stay at home), this accounts for much of it.
In terms of community transmission, even during a stringent lockdown such as the one we’ve had in the UK this winter, around half the workforce are travelling to work, while only around a third work exclusively from home. Add to that that many people still use supermarkets and other shops, and many children still attend school (even where the schools are only open for key workers’ children), and that’s a lot of social interaction. We also know from a major UK survey that less than half of people with Covid symptoms fully self-isolate, giving reasons such as going to work, going to the shops or regarding the symptoms as mild. This means we don’t need to resort to unsubstantiated ideas of asymptomatic infection being a major driver of transmission (which is unsupported by evidence, since, as with other similar viruses, asymptomatic carriers of the disease are barely infectious and contribute very little to spread) to explain ongoing community transmission.
Masks and distancing have little or no effect on transmission, mainly because they do not (and cannot, since people must breathe) prevent virus-carrying aerosols from filling the air in a poorly ventilated space such as most rooms we spend any amount of time in (we are after all trying to keep them warm). Breathing such air is likely the main mode of transmission.
There may be other factors too, but these are the main ones.
The game’s up. The data are in. Lockdowns are a failure as a tool of public health policy. Time to change the game.
Stop Press: Rowen Dean, editor of Spectator Australia, referred to our figures comparing the Covid death rate in US states that locked down last winter to that of the states that didn’t on Sky News Australia. You can watch the clip here.











To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.
“The important point is the big picture: the fact that in one big country with lots of different regions taking different public health responses, there was no obvious relationship between interventions and outcomes. “
That’s absolutely key. Unless lockdowns can be clearly shown to make a decisive difference, then, in scientific terms, the support for what was always an unlikely idea doesn’t exist.
For sure. And makes Boris Johnson out to be the bare faced liar we all know he is.
“it was the lockdown which brought the cases down”
Liar.
Trouble is, BBRC, is that millions of people believe him.
That is what politicians strive for and what they are paid to do. Our job is to say the truth, of the two measures that can affect infections (lockdown and vaccination) vaccination is best at present.
No substantive evidence for vaccines, either.
Again – the null hypothesis stands.
Vaccines for the over-60s, and that’s assuming proper vaccines, and not these experimental ones.
PHE would beg to differ based on an analysis of 300k subjects and follow-up. The degree of protection from vaccination from symptomatic disease is far from the null.
See the plot, the effect is obvious, no need for dumb-arse hifallutin Latin.
I fell off my bike ten days ago.
Since then, Covid infection rates and deaths have gone down substantially.
Behold, I can work miracles.
I’m sorry you fell off your bike, but it’s a stupid claim, missus, hence are we to assume you are stupid? Explain the link, or find a better theory.
If you need it explaining, you are the stupid one. Look at the definitions of correlation and causation, anybody with half a brain can see that the drop off in a seasonal virus is nothing to do with ‘vaccines’ or NPI’s.
*please note, I don’t think that Annie actually fell off her bike, probably apocryphal fellah.
Sorry you don’t understand standard English. Another item to catch up on.
“PHE would beg to differ”
How true that is. They’re into misleading – as noted by the CEBM, if you recall.
Just quote to me the ARR figures, that I’m sure they’ve published 🙂
For many reasons we use relative risk reduction. You’re obsessed with unmeasurable absolute values.
what about this for you null hypothesis, a plot assymptotically trending to zero? You think it’s just good luck? yeah right. You are demented with bitterness. No problem spurn the vaccine, and get lockdown, harder, longer, sooner…. you are the perfect author of your own misery, too stubborn/stupid for your own good.
Getting those blinding lights again where you can’t see anything but this monotonously repeated graph which simply describes the expected curve?
Which curve is interesting on the upward slope in suggesting that the introduction of the vaccines might well have caused a rise in mortality that may have actually delayed the natural decrease.
You are quite entitled to buy into the vaccine mythology that gives the Covidevils more power – but don’t expect others to do so.
Oh … and simple logic is another thing to try to get a grasp of. As well as the folly of resorting to ad hominem (now that is Latin) gibberish when you’re losing an argument. It’s always a tacit (from the Latin) admission of defeat or ignorance.
Earlier to-day you were claiming that self-imposed lockdowns had resulted in a 70% plus decline in the infection rate (See Oxford study post).
That, of course, was complete nonsense. There is no evidence that lockdowns have any more than a marginal effect on infection rates as we see from the US.
There are two measures that might account for it, lockdown, vaccination or both. It does not matter which dominates, and there is presently no way to tell anyway. if they work, I’m happy..if you’re not happy, too bad.
Neither lockdown nor vaccines can satisfactorily explain the 2 peaks or the subsequent declines.
1/ The declines began BEFORE lockdowns could have taken effect.
2/ This means that infection rate was slowing several days before that (dynamics of virus transmission)
3/ ZOE is useful as a leading indicator but it doesn’t capture hospital and care home infections which caused a big chunk of the deaths in Dec & Jan.
4/ The most reliable data are the figures related to DATE of Deaths since they are not influenced by scale of testing. This shows a peak on or about Jan 21st 2021 (using 7 day moving average) .
The Mean time from initial infection to death follows 2 Gaussian distributions, i.e. ;
Incubation Period ~5.1 days
Symptoms to Death ~17.8 days
Total Time ~23 days.
This puts peak infection at the end of December – possibly a bit later since many of the over 80s died following the Pfizer vaccine which significantly suppressed their immune systems.
Further to my other reply to you, Tim Spector (ZOE) actually supports my point about cases falling before lockdown. The UK introduced the second lockdown on Nov 5th. On November 6th, TS writes
https://covid.joinzoe.com/post/over-the-second-wave
Before every lockdown the “COvid death” curves were on a downward trend
“There are two measures that might account for it, lockdown, vaccination or both.”
Errr … So what happened in April 2020 when neither applied??????
> to what happened in April 2020 when neither applied?
in April 2020, the PM was in critcal care and 1,000 a day were dying with covid19.
If you look at deaths rather than infections then the decline last spring was almost as steep as this year. Obviously the decline last year wasn’t due to vaccines, so it makes no sense to claim this years decline was.
Yes – I’m afraid the key point was entirely missed. As usual. I don’t think the fact of a steep ‘unaided’ decline from a higher point in a similar curve was noticed, either.
Hopefully fon has had his jab just like a good boy should.
He / she will be dead within twelve months.
Enjoy it while you can.
I can show lockdown probabley did buy a very small advantage here, but at huge cost, not really worth it.
There are only two measures, lockdown and vaccination, both have some effect. Vaccination has the biggest effect now, in conjunction with better weather.
False dichotomy: there is another skywalker, sorry, way, the way in which we protected the vulnerable and took basic precautions, banning large indoor events but otherwise letting people get on with their lives like a liberal democrasy should.
you can vote on it…
No, we can’t.
Look at the graph. Read the article. Lockdowns don’t work to control the virus spread. They may temporarily delay it, that’s all, if everyone, absolutely everyone is confined to their homes, but you destroy the economy, people would die from other causes, and the virus would spread around again as soon as lockdown is lifted.
Unless you do what Australia and NZ did of course: lock down until the virus is eliminated (easier for them to do because seasonality meant it didn’t get very prevalent in the first place) and then seal the borders to stop it getting back in.
Most countries don’t have that capability though.
I vaguely aggree with that, it’s a good plot, but tells us little.
Unfortunately, that won’t change their minds, or stop them from imposing them again.
They’re not going to let data get in the way of a good narrative.
The plot tells us it’s not worth doing lockdown, but ut tells us that in a complicated way! It’s a good plot that tells us nothing. In conclusion, there appears to be no material difference between doing lockdown or not doing it, it is best to not do it since lockdown is disruptive. Two of the main things that differentiate various states are their relative populations and their climate. So let’s look at this graph, in particular the 4 outliers at the right which all did winter lockdown, and had high death rates, and the outliers on the left which did no lockdowns. Sometimes in statistics, the outliers tell the story.OK, first the high fatality outliers Rhode island, 1,057,125, climate cold Massachusetts, 7 m, cold New York 20m, v. cold (see midNight Cowboy) New Jersey, 9m, v cols (see above) So big populations, relatively, and all cold and damp (maritime). So no obvious answers leap out yet, so let’s see low mortality outliers Hawaii, 1.5m, v. warm. vermont, .6m, very cold Alaska, .75m, very cold Maine 1.3m, v cold So again nothing obvious. The size/climate number on the outliers do not give the game away. So I’m stuck. What IS going… Read more »
There is a real virus around, its called ‘fon’.
It’s harmless.
Well at least you’ve acknowledged this here. Elsewhere you blather on about lockdowns and vaccinations being the only two ways of dealing with disease. It’s obvious lockdowns cause at least as much damage in the short term as they prevent, and in the long term far more.
>lockdowns and vaccinations being the only two ways
please tell us the others.
Growing natural population immunity; seasonal effects – the basic nature of viruses.
The fact you even need to point this out to him/her/they demonstrates the worthlessness of continuing a discussion with him/her/they. I tried to yesterday, but it’s just a waste of keyboard time.
Fon has hit the bottle.
Hilarious.
There are two ways to deal with fon, who is clearly a 77 Brigade amalgam:
take the piss or ignore the dozy ducker.
Dr Fauci says the people in the states that locked down didn’t obey the lockdown. And he seems to think he is making a point in his favour by doing so, which is worrying.
And in the states that didn’t lockdown, people just did it anyway, more rigorously than the ones that had it but didn’t obey? amazing
Surely the main reason lockdown doesn’t work is that people with a high viral load generally feel pretty unwell so stay at home without being told to do so. Therefore anyone who feels well enough to go out is unlikely to be highly contagious and it’s therefore pointless to make them stay home.
Isn’t Oregon the state which kills old people?. If it’s the one I am thinking of, hospice care also suffered after this started. And now… you see where crimes against humanity lead.
Brilliant article on the US ‘case study’. I know nothing is really new but for the less informed these are the key arguments that go against the lockdown strategy as a viable or successful one. The real ‘negacionists’ are the ones (MSM/politicians/experts) who either don´t want to see this evidence or find funny arguments to, in desperation, try to counteract it. Trouble is: this is the REALITY and you cannot pretend it doesn´t exist!
The argument most people use against this kind of data is this:
‘Yeah but those states still had SOME measures like masks/social-distancing and without those? The deaths would have gone up! And if those non-lockdown states had locked? Their deaths would be even lower.’
‘And anyway the population density is different so you can’t compare them.’
Not my argument but it’s what people always say to me. People appear to not want to believe the counter arguments.
Not sure why I got downvoted for that. I’m just relaying what people say to me!