Now that Chile is settling down a bit, the latest Covid cautionary tale is India, which never seems to be out of the news at the moment as its positive cases and deaths have rocketed in the past few weeks.
Even the usually level-headed Kate Andrews in the Spectator has been painting the situation in lurid colours.
As it happened, the UK’s worst nightmares were never realised. The Nightingale hospitals built to increase capacity were barely used. But what the British Government feared most is now taking place elsewhere. India is suffering an exponential growth in infections, with more than 349,000 cases reported yesterday, as well as nearly 3,000 deaths. Hospitals are running out of oxygen for patients and wards are overflowing. There are reports of long queues as the sick wait to be seen by medical professionals. It’s expected the situation will deteriorate further before it gets better.
Jo Nash, who lived in India until recently and still has many contacts out there, has written a very good piece for Left Lockdown Sceptics putting the current figures in context – something no mainstream outlet seems to have any interest in doing.
Jo makes the crucial point that we need to keep in mind the massive difference in scale between India and the UK. At 1.4 billion people, India is more than 20 times larger than the UK, so to compare Covid figures fairly we must divide India’s by 20. So 2,000 deaths a day is equivalent to a UK toll of 100. India’s current official total Covid deaths of approaching 200,000 is equivalent to just 10,000 in the UK.
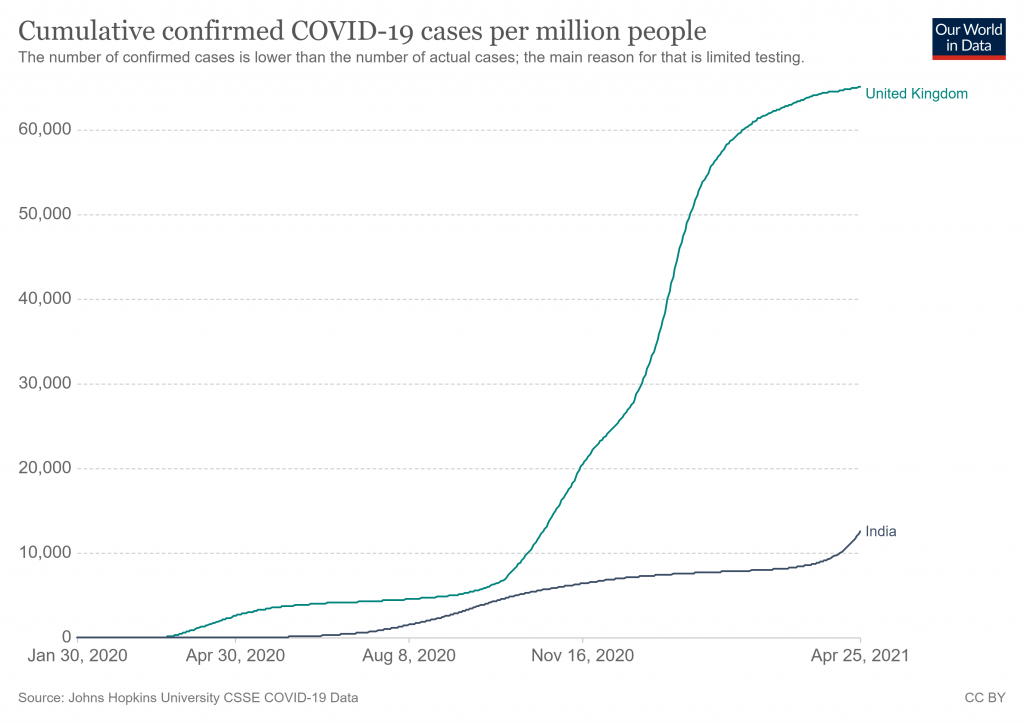
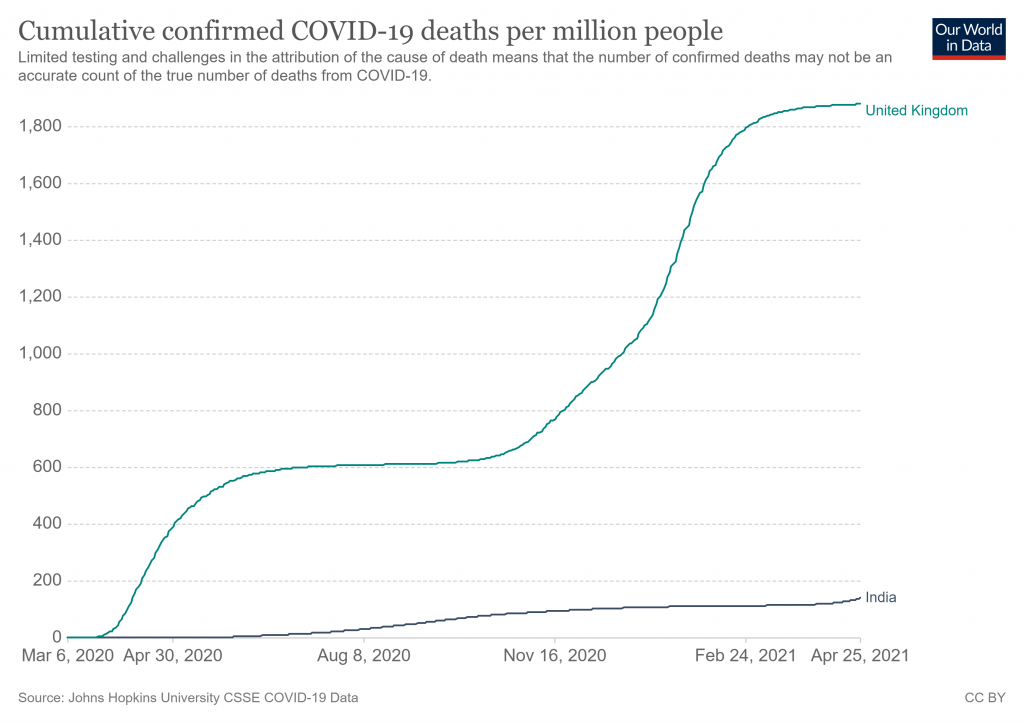
In a country the size of India and with the huge number of health challenges faced by the population, the number of Covid deaths needs to be kept in perspective. As Sanjeev Sabhlock observes in the Times of India, 27,000 people die everyday in India. This includes 2,000 from diarrhoea and 1,200 from TB (vaccinations for which have been disrupted by the pandemic). The lack of adequate hospital provision for Covid patients may be more a reflection of the state of the health service than the severity of the disease.
Jo Nash also points out that poor air quality plays a role.
Delhi, the focus of the media’s messaging, and the source of many of the media’s horrifying scenes of suffering, has the most toxic air in the world which often leads to the city having to close down due to the widespread effects on respiratory health…
Respiratory diseases including COPD, TB, and respiratory tract infections like bronchitis leading to pneumonia are always among the top ten killers in India. These conditions are severely aggravated by air pollution and often require oxygen which can be in short supply during air pollution crises…
According to my contacts on the ground, people in Delhi are suffering from untreated respiratory and lung conditions that are now becoming serious. I’ve also had breathing problems there when perfectly healthy and started to mask up to keep the particulate matter out of my lungs. I used to suffer from serious chest infections twice yearly during the big changes in weather in India, usually November/December and April/May. When I reluctantly masked up that stopped. My contacts have reported that the usual seasonal bronchial infections have not been properly treated by doctors afraid of getting Covid, and people’s avoidance of government hospitals due to fear of getting Covid. Undoubtedly, these fears will have been fuelled by the media’s alarmist coverage of the situation. Consequently, the lack of early intervention means many respiratory conditions have developed life-threatening complications. Also, people from surrounding rural areas often travel to Delhi for treatment as it has the best healthcare facilities and people can go there for a few rupees by train. This puts pressure on Delhi’s healthcare system during respiratory virus seasons.
Positive cases look like they may be peaking in many regions now.
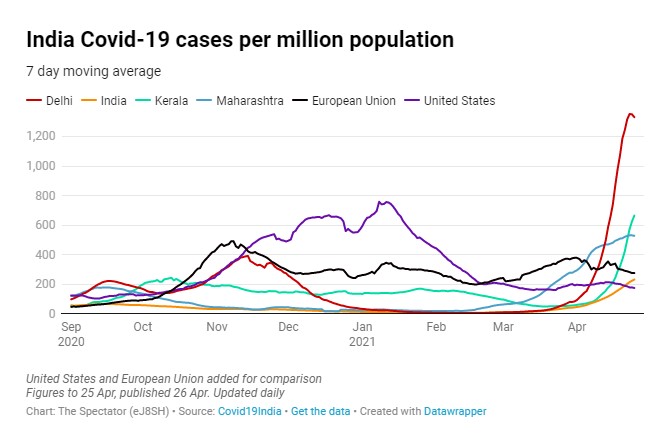
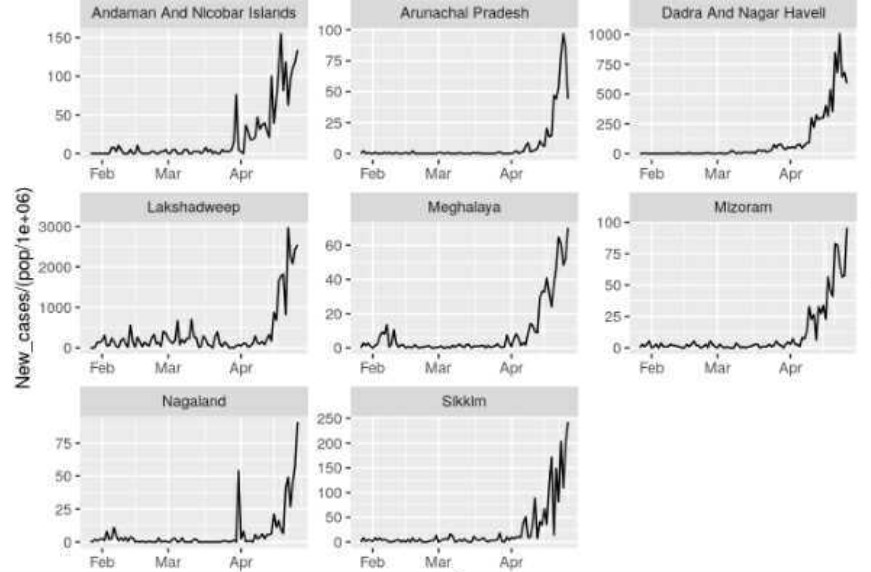
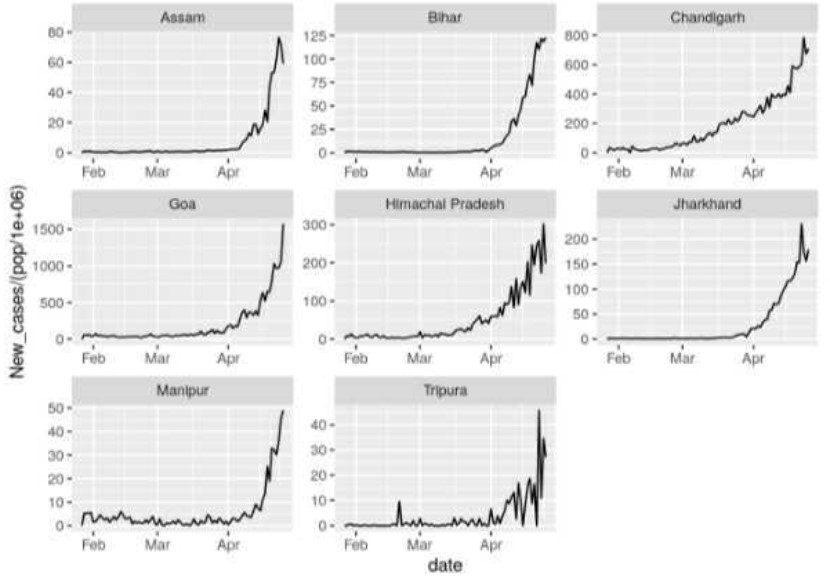
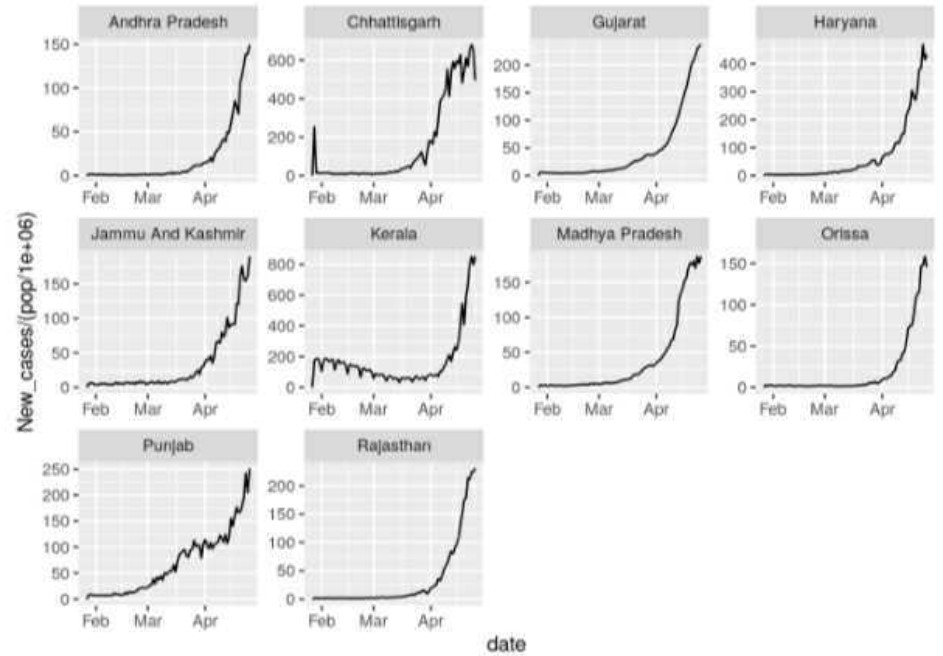
One mystery, as yet unexplained, is why India, which has not experienced a strong surge like this so far, suddenly did in March and April. Adding to the mystery is that the simultaneity of the surge across the regions is unexpected in a country as large as India and contrary to earlier outbreaks last year. Nick Hudson from Panda suggests it means there must be something artificial about it as it is not a natural pattern, since viruses naturally spread across the country with some delay and variation evident between regions.
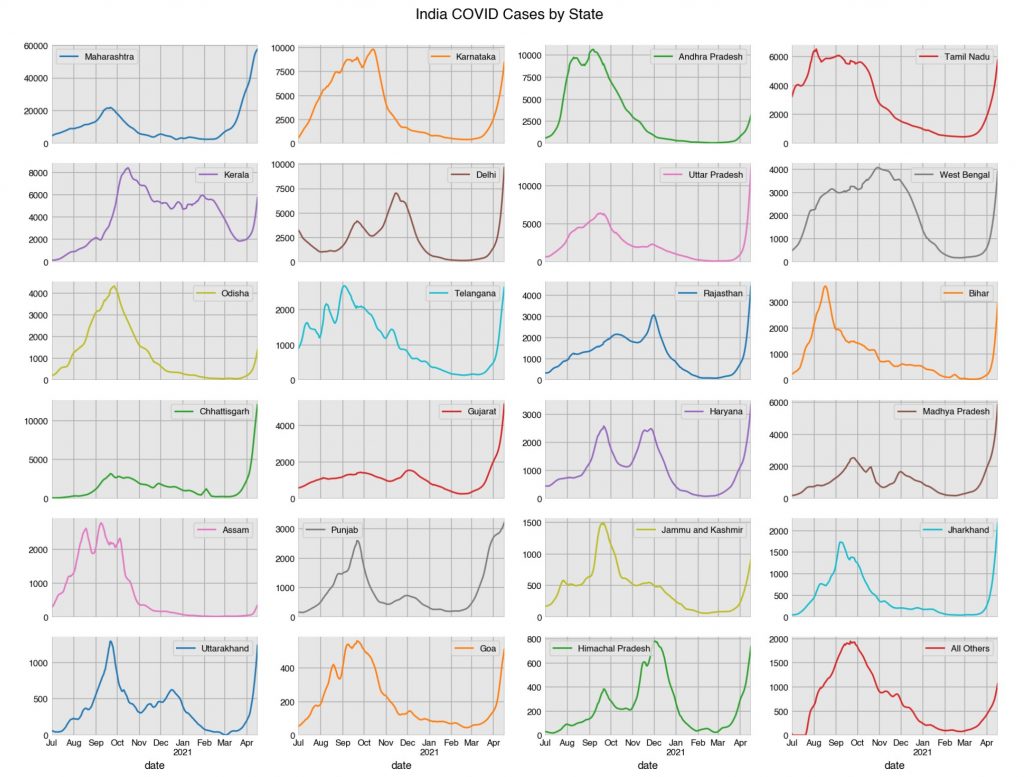
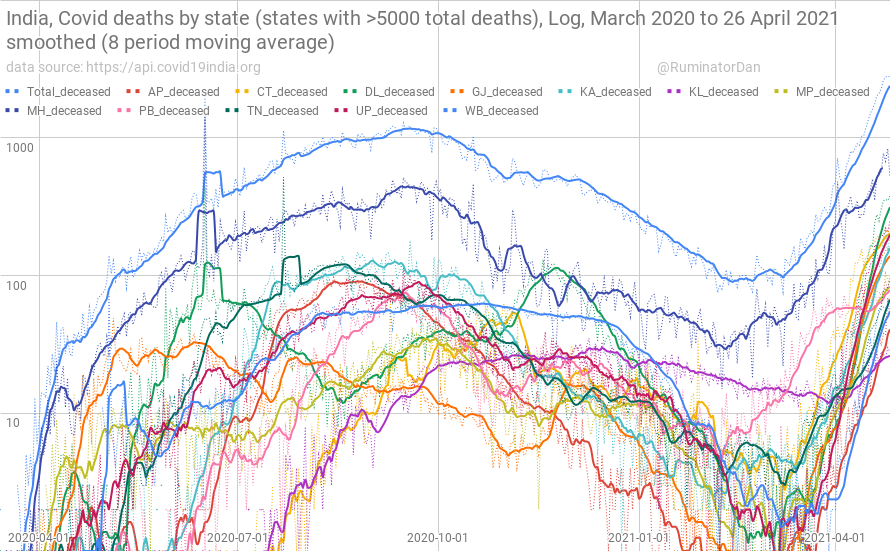
It hasn’t escaped people’s attention that one novel factor is the nationwide vaccine programme rollout, beginning in January and accelerating during March. Is this a further example of the post-vaccine infection spike seen in the various trials and population studies, possibly caused by temporary suppression of the immune system?
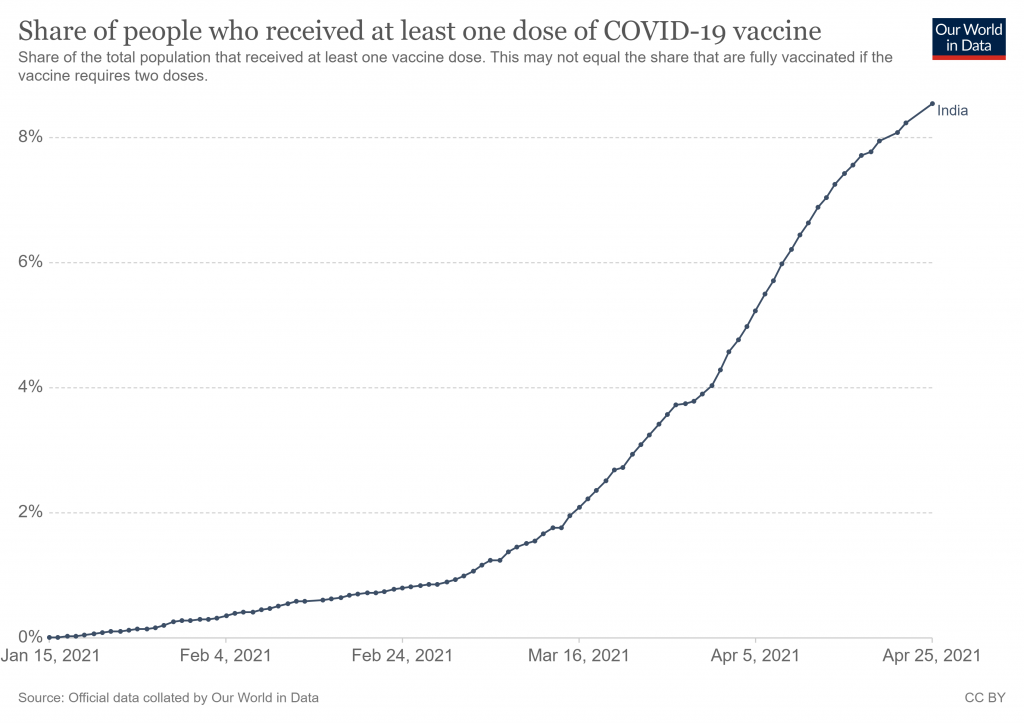

Testing is another possible factor, as the number of tests being carried out surged in March and April – though so did the positive rate, suggesting this can’t be the only explanation.
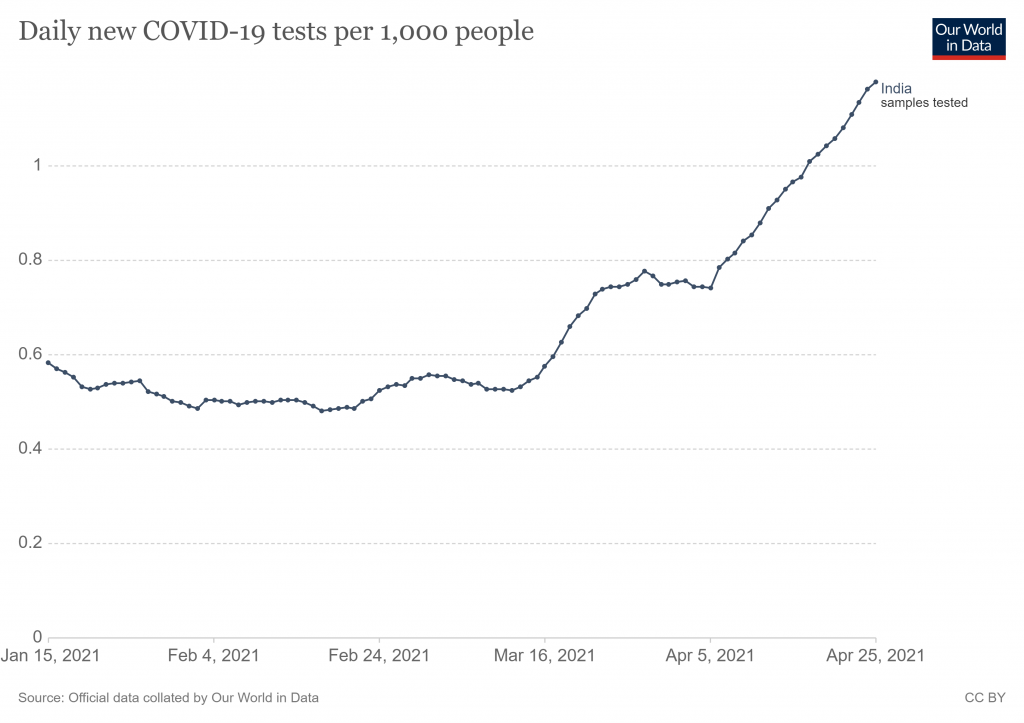
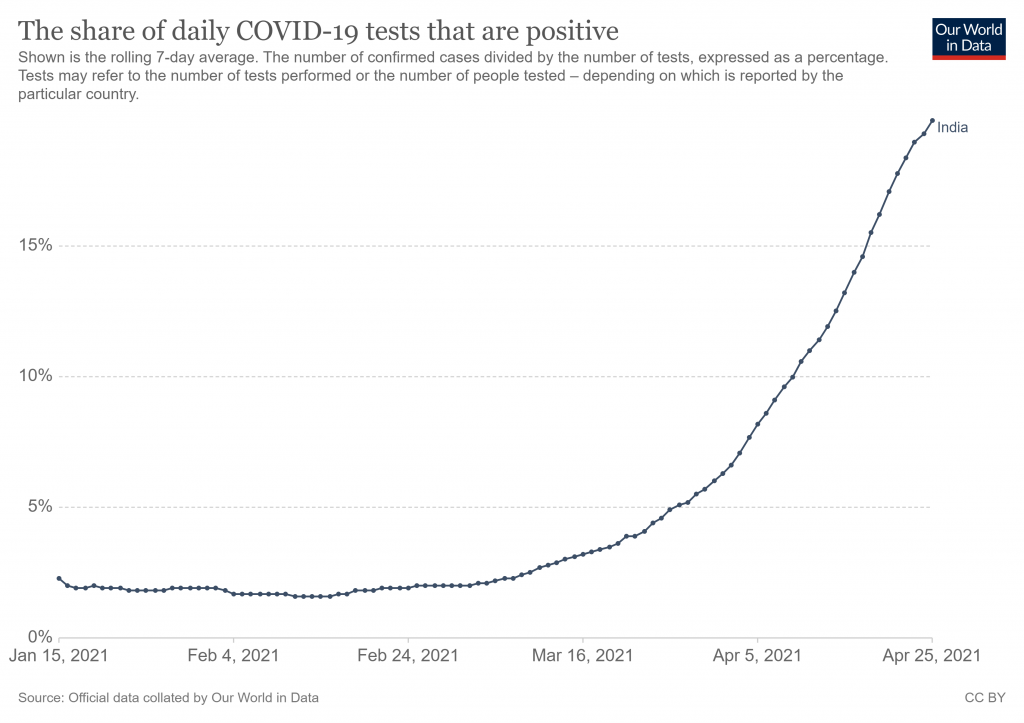
Whatever is going on, it’s a pity there is not more curiosity among our scientists and journalists. Instead, it’s just the usual scaremongering driven by the misrepresentation of data.
Stop Press: Former Assistant Secretary-General of the United Nations Professor Ramesh Thakur has been in touch with a comment he left on a story in the Australian.
Some context and perspective. India’s Covid deaths yesterday were 2,163 (seven-day rolling average). India’s average daily death toll is 25,000 from all causes.
Second, despite this surge, as of now India’s Covid mortality rate is 140 dead per million people. This compares to 401 for the world average, 1,762 for the US, and 1,869 for the UK. It puts India 119th in the world on this, the single most important statistic for comparison purposes.
Third, the crux of the problem in India is not the proportion of cases and deaths from Covid. Rather, it is the lack of a fit-for-purpose public health infrastructure and medical supplies of equipment and drugs.
Fourth, although Government neglect of public health while prioritising vanity projects like a new Parliament building during the pandemic, building temples and statues etc. is a contributory factor, the real cause of a poor public health system is poverty. Put bluntly, poverty is the world’s biggest killer.
Fifth and finally, this is why a strong economy is not an optional luxury but an essential requirement for good health.












To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.
Again, we see increases in deaths correlating with a vaccination programme. The temporary suppression of the immune system could be an explanation. However, we cannot be sure of the cause of death if we rely on the PCR test alone. And, if the deaths were covid-19 based, then the virus would need to be present and transmissible at each death.
In the UK, we saw a similar correlation, peaking a couple of weeks later than the customary seasonal peak. And the fatalities were predominantly the elderly (75+) in care homes. There would have been much safer environments there than in India. A suppresssed immune system would have been better shielded.
So it is looking to me that a more likely cause of death is a reaction to the ‘vaccine’ itself. For frail people, it is just too much. Something is unsafe. It seems not to be having such a serious effect on younger people, but ‘vaccine’ deaths currently total 973 and are running at 14 per day according to Yellow Card Reporting. And the government estimates that only 10% of serious adverse reactions (which I take to include death) are reported.
https://www.timesofisrael.com/israel-said-probing-link-between-pfizer-shot-and-heart-problem-in-men-under-30/
Should it not read “in morons under 30”? Who the F under 30 is voluntarily allowing dreck to be injected into their body?
On the other hand it does look like a concerted collective attempt to make it into the Darwin Awards.
The Israeli government isn’t making it voluntary. They introduced the covid pass to allow vaccinated people some former freedoms. That tends to exert unnecessary pressure on people to conform.
I still wonder if the huge spike in hospitalizations and deaths from November through early February might have been caused, at least in part, by a reaction to so many more people (especially the older, more at-risk populations) getting their flu vaccines during this period. I of course don’t have any data to support this possibility and this probably isn’t/wasn’t a factor in these massive spikes … However, I also know that this would definitely qualify as an “off limits” study. That is, this represents a hypothesis that “science” and researchers cannot entertain.
There is a thesis like this suggesting that is why the Bergamo area had it so badly in Italy – the elderly had just all been vaccinated against the flu!
Dr Zach Bush – Del Big Tree show
– should have taken people off statin based drugs, halted flu vaccines as they up regulate the ace2 receptors
Just listen to this woman and her problems – the same problems my daughter has in Florida with millions of other women all over the world. Just now making it massively into SM – without naming the cause, as this would lead immediately to blocking/removal of content. Strong nerves required.
https://rumble.com/vfz7rv-you-must-listen.html
Repost since it’s topical.
This from the Times of India shows the most common causes of death in 2020.
A ‘Lakh’ is 100,000 apparently so there at #7 is TB with 450,000 deaths or 1,200 a day as Will Jones says in his main text.
By far the biggest killer is heart disease with 1 million and 540 thousand killed per year or 4,200 each day which has not unduly worried HMG or our domestic press in the past.
Yes, anything that puts a situation in context is worth reposting. Had the fatalities last March/April been put in context, we would not be in the current mess.
… which is the main reason I got engaged in looking at basic data for myself last April : the pushing of data without context in the MSM smelt to high heaven of propaganda.
Of course – we were right, but even a year ago, people were already brainwashed and would not look at the reality.
It’s never been illegal in Britain for people to die in India – until now.
Despite the recent Billy Bunter nonsense, the UK government and its media hacks are for ever on the watch for new reasons to lock us down. India looks very promising to them.
Or simply to justify locking us down …
Yes.
The mainstream media is the equivalent of side-bar click bait. Minus the positive messages about stay-at-home mums discovering amazing cures.
There’s always a bright spot. Every time I go to Conservative Woman, I see an ad for a miracle cure for earwax. Just what the country has been crying out for.
That ad pops up everywhere. It’s absolutely gross!
Oh good, I was rather thinking it was just me !
I found one simple trick stopped a pandemic. I turned off the TV. Doctors hate me.
You’re right to point out, yet again, the corruption of language by Covid fanatics.
It isn’t entirely new, however. Years ago I saw a joke featuring an Irish minister: ‘Well now, if they say the figures are spiralling, isn’t that better than going straight up?’
Based on the 1.3 billion people in India it means they have an IFR of 0.0003%, fantastic, has to be the best in the world.
We need to copy them and do away with the NHS totally (health care for the rich only) and also most of our public sanitation(what did Dr Snow know) and plough that money into our Space Programme.
The IFR would be that if every one of the 1.3 billion had been infected. More context though:
‘The shortage of oxygen has nothing to do with covid . . . (But from) institutional and bureaucratic incompetence.’
Todays roundup (above) includes
“Wear masks even inside your own home”
Half of the article is an Indian government person explaining that there is no shortage of oxygen, the problem lies with distribution.
“ Perspective on India <200,000
In the EXACT time frame India has lost 809,000 people to Flu/Pneumonia (4X the deaths attributed to to COVID),they lost 537,00 to Diarrhoeal diseases,553,000 to tuberculosis.392,000 to traffic accidents, 283,000 suicides“
https://www.worldlifeexpectancy.com/country-health-profile/india
And then there’s the accidents with fire and exploding gas cylinders used for cooking!
“ 850 deaths out of 27,000 a day in India. And the pressure is for India to impose measures that will divert its limited resources from the expenditure on healthcare and sanitation that will actually preserve life, while depressing its economy and so starving its poor. “
(Source: https://threader.app/thread/1386740108351741954)
“Yes, 850 died of covid recently in a day, but 27,000 die every day in India”
https://timesofindia.indiatimes.com/blogs/seeing-the-invisible/yes-850-died-of-covid-recently-in-a-day-but-27000-die-every-day-in-india/
Far too much sense in that article. Had to be balanced by your usual bedwetter commenting:
The logic of this escapes me. Why would it be morally wrong and insensitive to compare old people dying of covid with old people dying of other things?
Life in the West is one great lie at the moment.The mainstream media is the chief liar. I look forward to its demise.
Indeed. In the meantime, I would suggest that the best source of impartial, honest reporting is UK Column News which deserves all our support.
Homepage | UKColumn
Unlikely, given how many people drink it all in.
Caitlin Johnstone just penned another provocative column. In this one she posits that the mainstream media is simply doing its intended job. And the “mainstream media” is not going anywhere (the role it plays is too important). That is, the journalists in these newsrooms will continue to practice “pack journalism,” which ensures that dubious narratives will continue to be perpetuated, protected and advanced.
It would be nice to think we could “drain the newsrooms” when we “drain the swamp” (the former is actually a prerequisite for the latter) … but this isn’t going to happen.
The best we can hope for is that more “contrarian” sites like this one are created and find a significant audience.
And me
Latest data shows the death rate in India is:
Is it worth mentioning that the whole India thing is mainly a lie and a psy op? They have been using old photos of a gas leak from May 2020 where a few people were lying ill outside the building and they are using the same pictures for the lastest ‘Covid crisis’.
So if my calculations are correct Covid is responsible for 3% of the daily deaths in India. (850/27k x 100 = 3.1%). What ever happened to the 500000 we were told will die in the first wave.
I was looking on OurWorldInData at the India data.
Their vaccination programme really got going in volume on March 28th. Huge increase started on that day. Daily vaccinations went from about 400,000 to more than 4 million.
On March 29th, daily deaths in India were 271
Three weeks later they were 1761.
We have seen this coincidence in many countries now. Gibraltar, UK, Israel, Seychelles, now India. It’s starting to become a pattern.
It is certainly as likely as ‘the vaccine has cured us’ mythology. But I reckon we have to be careful of doing our own riff on confusing correlation and causation.
I won’t have a vaccine – and that possibility is one of the reasons – which is why I’ve reacted strongly against the endorsement here of the idea that ‘It’s OK for the vulnerable’.
Of course correlation is not causation. But as I mentioned, the fact that this has happened in multiple countries now makes it at least worthy of study.
What will be interesting to see is what happens if and when vaccination really gets going in a country where there is little or no live virus – e.g. NZ or Aus.
I suspect the issue here is rolling out a vaccination programme in places where there is still a lot of “live virus” around, and the combination of having both the virus and the vaccine sends many people over the edge.
If that is the case we should see fewer deaths in NZ and Aus.
“worthy of study”
I think I’ve implicitly agreed with that. What I’ve said is that at present., it is a credible hypothesis rather than a firmly established concept.
My caution derives simply from a recognition of the need to be scientifically precise and clearly distanced from the sort of fictional crap that the propaganda is using.
Agreed.
I wonder if there’s an element of obesity mixed in here. Those who can afford any sort of hospitalisation in India are likely much more westernised and India has some of the fastest growing rates of obesity of any country.
Yes, Dr Aseem Malholtra recently highlighted this link. Indians are actually in very poor metabolic health and lacking in Vitamin D as they want to be as white as possible…
Thanks for that – although quoting data on ‘cases’ is questionable.
Somebody asked me about the situation in India, and I had to confess that I hadn’t looked for accurate information, although I knew that the MSM coverage woukd be diversionary propaganda. A quick look at Worldometer data (even with its inherent flaws) quickly showed how deaths in proportionate terms were wildly exaggerated – with India way below the UK, at about 118 of all countries.
The gap between the MSM and reality is now becoming more and more absurd. Decent reporting almost a vanished art.
The “groupthink” in newsrooms on COVID topics approaches 100 percent. It’s thus almost impossible for these journalists to produce articles that would challenge the ‘conventional wisdom” on COVID topics. I have noted that the UK press produces more stories that might qualify as broaching “off limits” COVID topics than the U.S. press.
“Pack journalism” is a more ominous “disease” than COVID-19 imo.
Well summarised.
I found this story from a Florida newspaper (picked up nationally by the Drudge Report) more confusing than illuminating. https://www.sun-sentinel.com/coronavirus/fl-ne-south-florida-covid-hospitalizations-continue-20210424-jxuqa5zerfc2lfaturmabsbke4-story.html The story purports to show/suggest that new variants have caused hospital admissions in Florida to rise. The article states that virus “variants” are much more prevalent in the 25-to-44 age cohort, but the story provides no specific data that provides the (absolute) number of 25 to 44-year-olds with COVID who are currently hospitalized. (The story does note, in general language, that those who have contracted the variants aren’t being hospitalized, or this seems to be implied). To better support its conclusion, it would have been nice if the article’s author included information on actual hospitalization numbers by age cohorts. The article does tell us that “As of Friday morning, about 3,500 people were hospitalized for COVID in Florida.” This is good information, but it would also be good to know the age ranges of these 3,500 hospitalized patients and the actual numbers by age cohorts. Of these 3,500 patients, how many are under the age of 45 (the age most susceptible to variants)? How many are over the age of 55 (the group most likely to have been vaccinated by… Read more »
The above-linked story also states that 25 percent of Floridians have been “fully vaccinated.” It also includes this quote from a doctor “…. we’ve done an amazing job vaccinating people over 65,” (the doctor) said. We also learn from the story that “most” people who have been hospitalized (with or without “variants”) are people over 55 and we know that Florida has done an “amazing job” vaccinating people 65 and older … but still those being hospitalized appear to be disproportionately from older age cohorts. I would think by now that perhaps 80 to 90 percent of Floridians over the age of 65 have been vaccinated. If this age group STILL makes up the vast majority of hospitalized COVID patients, can we make logical conclusions that speak to the “effectiveness” fo the vaccines in preventing “severe” cases (those that lead to hospitalizations)? It seems to me there might be some kind of journalism conspiracy to NOT report the ages of hospitalized COVID patients, and/or what percentage of these older hospitalized patients had already been vaccinated. Is the point the author and authorities trying to make this: That older people are still being hospitalized from COVID at disproportionate rates … but… Read more »
The lack of interest across govts, media and public health bodies in simply finding useful data to learn more about covid has been astonishing
You’d think that such a new, deadly threat would have people making every effort to understand it more, but that’s not been the case
Yes!
Once the original “modelling” was produced, that is what has been and is still being followed. Facts are irrelevent.
Lots of excellent questions in the original article, yet who would look at vaccinations or air quality just for two
Where are the journalists or editors in these newsrooms who would “call out” these inflammatory (and non-sensical) headlines? There are none. They all agree with these characterizations. … So nothing is going to change. In fact, things will only get worse.
XR is establishment astroturf.
BBC Radio 4 news at 12 has just led with the headline ‘there are fears that deaths could be being under-reported and may be twice as high’ or words to that effect. Give. Me. Strength. .
“there are fears that” = It suits our narrative for people to believe this is the case
Even if they were twice as high they would still be unexceptional
Just heard that whilst on M40 🤦🏼♂️
My son informs me that there was a gas leak in India last year which killed a number of people and the video footage showing the covid bodies is from then. He also said that an Indian person who lived near one of the sites where there are supposed to be piles of covid victims bodies and he blogged there was nothing there.
I haven’t personally seen any reported evidence as to whether this is true or not, other than taking my sons word for it. Can anybody corroborate this story?
Someone posted this link elsewhere BTL
https://twitter.com/mrgeckouk/status/1386983340889280515
Appreciate the image to the article. For years (as an asthmatic person) I have been pointing to toxic air pollution being the greatest killer of them all. In 2019, ~4.5 million people died of respiratory failure due to particulate matter smaller than 2.5 micron. Also referred to as “Nano Particles” and their origin is absolutely not limited to volcanic eruptions, forest fires, burning oil fields and industrial pollution. The de-populaters add millions of tons of nano particular matter into the upper atmosphere.
The hypocrisy is the faking concern about the health of people regarding a non-existing ‘virus’, while the real culprit is knowingly not mentioned. To verify my assertion, please visit once more:
ventusky.com “Air Quality” tab “PM 2.5”
Use the “play” button to have predictions at three hour intervals. Look at India and find other places with high
covidPM 2.5 fatalities.Totally agree! Air pollution is the killer not Covid. But given the lack of a vaccine to stop the transmission of air pollution, they will ignore it due to the ‘non-profitability’ of sorting this one out.
This article makes more sense than the propaganda from the MSM. It’s made zero sense for there to be a sudden massive surge of CV19 cases and deaths in India right now, but the air pollution, seasonality of respiratory infections at this time of year, a poor healthcare system, etc, makes more sense.
I believe that one reason India is actually doing much better than the media makes it out to be is the widespread use of Hydroxychloroquine and Ivermectin.
https://roundingtheearth.substack.com/p/the-chloroquine-wars-part-xvii
Given the wide misattribution of deaths in UK to Covid rather than the underlying conditions, I cannot think that India is any better at identifying Covid rather than pollution related effects as the cause of death. As the writer observes this is the time of year when pollution is at its worst, hence, possibly, the synchronicity of the disease around the country.
At last common sense. Where has the sensible journalism gone? Silly use of percentage increase when comparing vastly different populations and absence of infection mortality figures is scandalous. Where are our SAGE advisors to correct the errors?
Our SAGE advisors are so ignorant they couldn’t recognise an error if it smacked them between their eyes
The comment about air pollution is pertinent. In Delhi, the 2 largest components of air pollution are (1) road dust at ~35%, then (2) exhaust particulates, which are emitted from the mass fleet of very old diesel trucks and buses. Resurface the roads and properly maintain and renew the very old diesel fleet, and you will make a massive improvement to air quality. If there’s a case for masks there, it’s to protect against dust and particulates, NOT for the virus.
The real reason this totalitarian government wants to propagandise India, is so we go into yet another lockdown through project fear and hysteria. So far the SMEs have outsmarted the globalists and managed to maintain a presence on the internet. The government needs to create more furlough in order to completely bankrupt the country and destroy whatever is remaining of the entrepreneurial sector in order to bring in a ‘solution’. That solution is mandatory vaccination, universal income and population control.
Until the media start being honest and bringing this discussion to the fore instead of skirting round it, the country is heading for a total collapse.
You can’t bankrupt a country.
That spike following vaccination programmes seems to be seen everywhere. Once you see the lines plotted side by side, you cannot unsee it.
Thanks to Professor Thakur for the context