A new study of Covid hospital patients has found once again a spike in infections post-vaccination – what the authors call “an abundance of patients admitted to hospital within seven days of vaccination”.
The ISARIC4C consortium’s COVID-19 Clinical Information Network (CO-CIN) enrolled 52,280 Covid patients who were admitted to hospital between December 8th and April 10th. Of these, 3,842 had received at least their first vaccine dose, which is 7.3% or one in 14.
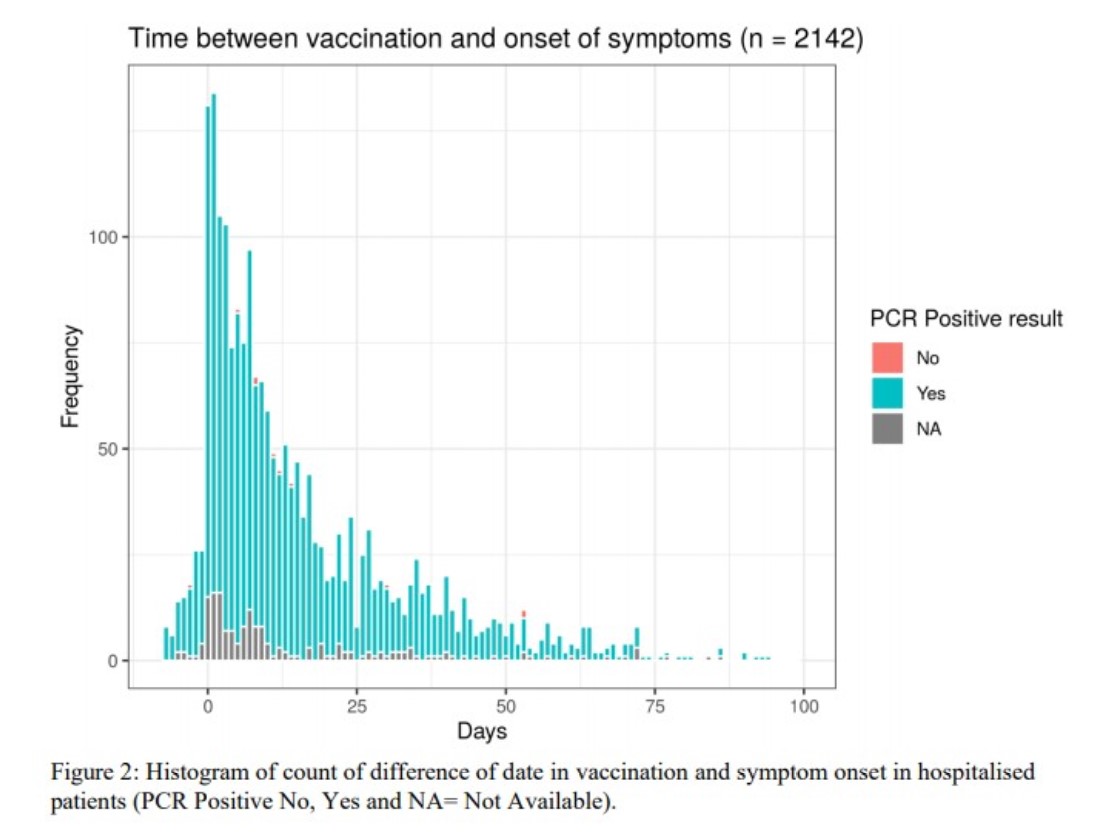
The researchers found that the median time between receiving a first jab and the onset of Covid symptoms was nine days. Since the median time from infection to symptom onset is five days, this suggests the majority contracted the disease in the days after vaccination.
The graph above shows how many of the vaccinated Covid patients experienced symptom onset on each day since vaccination. Note the massive spike on the day of vaccination and the three days afterwards. Although the authors do not say it in so many words, clearly the vaccines here are bringing on the symptoms. Why else would the frequency of symptom onset increase by 400% from the day before vaccination to the day of vaccination and in the following days?
The authors offer a few potential explanations. They suggest elderly and vulnerable people who had been shielding may have become infected through the exposure involved in the vaccination programme. Or perhaps they stopped shielding or being careful as soon as they got vaccinated, wrongly assuming they were immune.
The authors also raise the possibility that recent asymptomatic or mild COVID-19 could be triggered by vaccination into “symptoms likened to COVID-19 symptoms including fever”.
The study’s co-lead Dr Calum Semple, Professor in Child Health and Outbreak Medicine at the University of Liverpool, was clear where he stood on this, saying that the spike indicated “people are letting their guard down because they’ve been vaccinated. There is evidence here that people are unfortunately assuming that they’re protected very quickly after vaccination and that’s not the case.”
Such behavioural change was likewise blamed by Michael Day writing in the BMJ in March. Dr Clare Craig wrote a thorough riposte in the same journal, pointing to ONS data showing that the vaccinated did not increase their social contact and asking how it would explain similar spikes in care homes. She suggested other explanations were more likely, such as a drop in white blood cells in the days after vaccination as observed in the Pfizer trial, which may temporarily suppress immunity.
The spike in symptomatic Covid from day zero plainly cannot be explained by behaviour change, and as the authors suggest looks very much like the vaccine somehow re-triggering an old or existing Covid infection.
The good news from the study is that the vaccinated did not make up a large proportion of those hospitalised with Covid during December and January, though by late February and March (when all the over-65s were vaccinated) they made up a sizeable chunk of a much reduced total.
The authors note that the first dose of the vaccine doesn’t appear to reduce death among the high-risk hospitalised, saying “mortality appears to remain high for people in high-risk vaccination tiers who are admitted to hospital with symptomatic SARS-CoV-2 infection (COVID-19) despite vaccination 21 days or more previously”. It is not clear if this is a temporary effect owing to adverse effects of the vaccine or a permanent gap in the protection it offers.
How much longer can governments and scientists ignore the evidence of the post-vaccine spike in infections, found in study after study? When will they stop lazily blaming people for getting themselves infected and commit to investigate it properly?










To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.
It wouldn’t be a” temporary effect “ if it causes death!
You get jabbed, you get Covid, you die, you get your second jab, you rise again. Them snake oils is miracle cures.
PS. nice to see a bit of vaccine scepticism possibly creeping in here.
The worst hesitancy is unwillingness to see what has been evident to the wide awake from early on: that a proportion of those vaccinated die shortly thereafter.
And an even greater proportion after the 2nd dose will likely die in the middle to long term from effects ranging from anaphylaxis to the immune system turning on the endothelial cells, to the mass-produced spike proteins themselves disrupting ACE2 receptors and damaging mitochondria, to ADE.
“For if one drinks much from a bottle marked poison, it is almost certain to disagree with one sooner or later.”
https://bakerstreetrising.home.blog/2021/02/15/covax-through-the-looking-glass-part-4/
This ties in with the US study of the introduction of covid protein spikes into mice, which found that within 72 hours, they all experienced lung damage through inflamation. (28 April update).
If this is happening in humans as well, then those whose lungs are already compromised would suffer extreme effects. It would explain why India has been so badly affected since mass vaccination started, since TB and air polution have already caused major issues. It may well be why so many are dying within days or weeks of the vaccine being adminstered in this country too, particularly in the elderly, where so far, everything has been blamed on covid because everyone is too scared to blame the vaccine.
But has India been ‘so badly’ affected?
The last time I looked (1min ago), India is some way below the world average in and even ‘cases’ per million, and still not even in the first 100 of countries!
Ivor Cummins on India
(1) Short Video on India Situation: What does the Current Data Say? – YouTube
Spot that first wave that the MSN imply
Yep read this story, and was immediately drawn back to thisstory
Coronavirus Spike Protein Alone May Cause Lung Damage – Lockdown Sceptics
“This ties in with the US study of the introduction of covid protein spikes into mice, which found that within 72 hours, they all experienced lung damage through inflamation.”
So you’re a mouse, not a man?
What better way to “prep” your lungs for the damage than to wear a soggy, filthy bit of cloth over your nose and mouth for a year.
Try washing it.
You sound like one of those believers in “magical thinking”.
“People are letting their guard down…..”
Translation – it’s their own fault, trying to deflect the blame. Typical ploy of abusers everywhere.
How will we deal with 1000s of traumatised vaccine adminstrators when it finally dawns on them what they have done?
…prison terms?
…firing squads?
My mother told me she was ‘stewarding’ at an injection centre. As she is fully bought by Johnson I decided not to tell her she may as well direct the recipients to the gas chamber.
I am finding it difficult keeping track of which victims we are allowed to blame, and which ones we aren’t.
Just like all those women throwing themselves down stairs.
Last sentance adjusted ‘When will they stop lying?’ Answer, never.
Traditional vaccines use a weakened version of the live virus. This tells our immune systems we are infected, thus causing our immune systems to produce defensive antibodies. If we were PCR tested, we would of course test positive because we had been injected with the coronavirus, albeit in a weakened form.
MRNA vaccines are different, but is our response to them capable of triggering a positive test? I simply don’t know. Does anyone here know?
The PCR Test in particular has been so undermined that rather than be unfit for purpose it should be abolished.
Not ‘abolished’ – just properly used for the purpose for which it was designed.
Archaeology wasn’t it?
(1) All Types of COVID-19 Vaccines, How They Work, Animation. – YouTube
Depends on what segments of RNA the PCR test is looking for.
“MRNA vaccines are different,”
Not really. They just cut out the middleman of having to use a virus shell do the mRNA bit. The effect on antibodies is the same – because Coronavirus are RNA viruses.
Both attenuated RNA viruses and mRNA tech deliver RNA strands into your cells and co-opt the replication mechanisms within your cells. That then triggers an immune response.
You may well be correct, but the CoViD-19 mRNA injections encode purely (or so we’re told) for the spike protein, not the virion. They are training immune systems to have a very specific focus upon one small part of the “wild” virus. This is not the case for a “traditional” vaccine.
The AstraZeneca and Johnson & Johnson injections are “viral vector”. These are, also, nothing like a “traditional” vaccine, and they, too, encode purely for the spike protein.
So, you can, I think, reasonably argue that the mRNA injections are little different from the viral vector ones. Neither type should be touched with a barge pole!
It depends on the test.
Last time i checked in the UK our test was looking for 3 genes, only one of which was the spike and it required more than 1 to class a test as positive.
At worse a few days after vaccination could maybe trigger a spike gene but not the other 2 (as they aren’t included in the vaccines).
That said i did see an article a while back claiming LH labs were using a single gene hit as a “positive”. If true its (i) against all guidance and procedures and (ii) could do it.
That said, given where swabs are taken from, its incredibly unlikely even then.
I just cant see it.
It is the 1st of May and still the criminal charade continues…
Maybe this will be the month when the mass of humanity wakes up and realises what is being done to them? One can only hope.
Haha: for a second I thought that you were being serious!
Listen to interview with Dr Bhakdi and be chilled, as he explains in simple terms what the messenger RNA gene therapy vaccine does to your system. Search ‘New American Dr Bhakdi, using a VPN as it’s been banned in UK, if you can believe it. Staggering how the views of even microbiologists are censored if they run counter to the offical agenda..
You can view it here:
https://www.bitchute.com/video/FremXKQLjHJM/
I have found a number of articles reporting interviews with Dr Bhakdi using Ecosia as search engine 🙂
Bonus is that searching on it raises funds to plant trees in areas around the world subject to deforestation
I watched Bhakdi in spring last year, as a German I had the “privilege” as he was not being interviewed widely in English then, and I have been aware of his warnings about mRNA since then.
He was one of the first to speak out, trying to explain it in simple terms, and I encourage everyone to watch, read his information.
It’s funny how every case, death and wave is the public’s fault isn’t it? Trapped in an abusive relationship anyone?
At first-dose vaccination they should give a handout explaining that immunity is not instantaneous.
They do.
And its explained verbally.
What they should tell you is (a) your immunity will be reduce to all infections after vaccination, including Covid, for a period of at least a week and due caution should be exercised (it would be best to shield for a week minimum) and that (b) vaccination does not
guarantee long term immunity from Covid infection (even the manufacturers don’t claim that). To say it is not instanteous would imply otherwise – suggesting that all who are vaccinated do eventually become immune to Covid.
“ (a) your immunity will be reduce to all infections after vaccination,”
Why would they say that where there isnt a shred of peer reviewed, valid data showing that to be the case?
The data sheets make no claim over long term immunity either.
People don’t listen. Same as they don’t walk around with N95 masks permanently attached.
As ever network effects dominate. Which is why lockdowns and masks don’t work when they belief and the plan makes contact with the enemy of the real world.
How does Toby feel about this? He’s promoted vaccination as the way out of lockdown. What we see in actuality is that vaccination, particularly as it’s carried out over best part of a year, helps keep the “pandemic” going (diminishing though over time as you get to younger age groups being vaccinated I would accept). However, as other countries are just beginning their mass vaccinatino programme, we see that impacts on travel and allows SAGE to argue for continued lockdowns because of the “threat” of new variants from abroad,
“What we see in actuality is that vaccination”
Yes. Millions of people with jabs and it’s all working as expected. That’s the actuality of vaccination. The real mystery is why there are a mob of irrational people on here still trying to pretend it is anything other than a fantastic success.
They are indeed first generation vaccines, and they are not as good as vaccines for other diseases. But they are far better than the risk from Covid itself for the majority of people.
And that’s the choice we have – the disease or the vaccine. There’s isn’t another option.
Have you not read the stats. You have a 99.9% chance of recovery from COVID for those under 60. Those over 80 with severe comorbidities are at risk. Why in the helll do you think kids, young adults and even middle age people should take an experimental vaccine they do not even need. No long term safety or efficacy data, still in trial not finishing til 2023. You would have to be mad to take such an unknown. And knowingly giving it to kids and young people is criminal. Doctors and governments will be in court very soon for crimes against humanity. Shame on them
There are so many other options that I have lost count now – nebulised peroxide, HCQ, ivermectin, to name but 3 and if instead of the ludicrous and dangerous vaccination campaign the government had prescribed good levels of vitamin D to the whole country the pandemic would have been eliminated without the harms having been done by the vaccinations and no need for lockdowns. So it isn’t, as you say, ‘the disease or the vaccine’, it could have been the disease or the manifold other options, but these were at best dismissed and at worst supressed, with those using them in treatment threatened with the removal of their medical licence if did not desist with those treatments. BTW, just so we are clear, I am not replying to you – I am merely putting this up here so that anyone else who comes along and thinks that your “vaccine is all” strategy is accurate they will then see a more balanced and rounded view of what is going on with the state of medical treatment in this country.
Agree completely. It is an absolute disgrace that treatments that could have saved many lives, and still could, have been suppressed.
Posted by Simone Gold, America’s Frontline Doctors.
Dr. Vladimir Zelenko, an early adaptor and pioneer of the HCQ protocol, has been nominated for a Nobel Peace Prize.
This is the same doctor Twitter censored & banned from its platform.
His treatment has saved hundreds of thousands of lives. Well deserved,Dr. Zelenko!
The absence of adverse reactions does not mean ,or imply, that the treatment is working.
What absence of adverse reactions?
You’ve not been listening.
If this site has achieved anything its to point out the overblown reaction to a disease with an IFR of 0.15%.
A disease quite possibly derived from a lab leak.
https://www.nytimes.com/2021/03/04/health/covid-virus-origins.html
And the efficacy of the vaccines has been gamed, and the trials compromised by removing the placebo groups, and ignorance of pre existing immunity, and T cells, it goes on.
And you want us to put up or shut up?
We have the choice of the disease? Where from? For those of us with a well-functioning immune system, it would be worth queuing for. Such an option would reduce natural immunity hesitancy, as we could avoid the genuinely at-risk for the required length of time, right from the moment of infection.
The study’s co-lead Dr Calum Semple, Professor in Child Health and Outbreak Medicine at the University of Liverpool, was clear where he stood on this, saying that the spike indicated “people are letting their guard down because they’ve been vaccinated. There is evidence here that people are unfortunately assuming that they’re protected very quickly after vaccination and that’s not the case.”
Well that’s a load of BS designed to protect Big Pharma from an academic scientist isn’t it? Outrageous he thinks he can get away with that. Did people suddenly start leaving care homes for a night on the town? Absolute rubbish. And in my experience older people not in care homes have still been very cautious about their contacts.
Semple is among those who, early on, was wringing his hands about whether those recovering from Covid would be immune & if so how long would it last?
I looked him up to find he’d trained under a colossus of British immunology, Ivan Roitt, who wrote the textbook all U.K. biological subject undergraduates would have owned.
So I knew he was lying.
“When will they stop lazily blaming people for getting themselves infected and commit to investigate it properly?”
Occams Razor.
They are going to a vaccination centre where lots of other people are or have been, and they pick it up there. Symptoms within the first three days are vaccine side effects. After that it is overtaken by people who have picked up the actual disease.
The people in the vaccination centre are vaccinated and immune – so remain unaffected.
There is far too much default to ‘asymptomatic spread’, which is this particular diseases ‘ether’ or ‘dark matter’. The wardrobe monster that cannot be proved is actually there.
Poor show, 77th.
Ha ha, indeed, poor show. Your wily words are wasted.
Are you Fon’s mate by any chance?
That was meant for Lucan Grey btw
You shouldn’t be promoting an experimental vaccine that is still in its testing period. People aren’t guinea pigs. Go away
It would be interesting to see if there is any correlation between occurence of severe adverse effects immediately after vaccination and areas of high air polution or respiratory illnesses. Is the vaccine aggravating already compromised respiratory systems to a point of overwhelming it.
There is nothing unusual at all happening in India. What we are hearing is pure propaganda which is being foisted on the easily misled Western media consumers in order to manufacture rationales for massive vaccine dumps that will be subsidized by taxpayers. The funeral pyres in India are normal. This is simply how the Hindus do it- mass cremation. There are relatively few burials in India and based on tradition there have not been for say about several thousand years if not forever. Hindus cremate- Christians bury. India is majority Hindu and in poor areas there is mass cremation. The CNN’s, BBC’s of the world are counting on the Western media consumers to know nothing about the religions, traditions or culture of India. There is nothing going on in India other than increased testing with the phony PCR tests, fear mongering and priming the pump for a vaccine dump. Oh and mass repression deprivation by the Western-backed Modi government. The uptake of the “vaccines” was around 2.5% in India, not meeting the expectations of the Pharma ghouls, and the uptake in Western countries is stalling. This translates into massive numbers of pre-produced poisonous vials… Read more »
The spike in reported symptoms following vaccination can easily be explained. No one with recent symptoms is allowed to be vaccinated. So the period following the vaccination you will get symptoms from a combination of:
* people who were infected prior to vaccination but only now showed symptoms
* people who had symptoms prior to vaccination but deceived themselves or lied because they were so keen to be vaccinated and only admitted to symptoms afterwards
* people who mistook post vaccine symptoms for Covid symptoms (less likely in a group who ended up in hospital but possible)
All of these are going to add up to a “spike” compared to the period before when, if you were vaccinated, you should not have had symptoms, and the period after when the vaccine kicked in