by Professor Norman Fenton, Dr. Scott McLachlan, Professor Martin Neil and Dr. Magda Osman
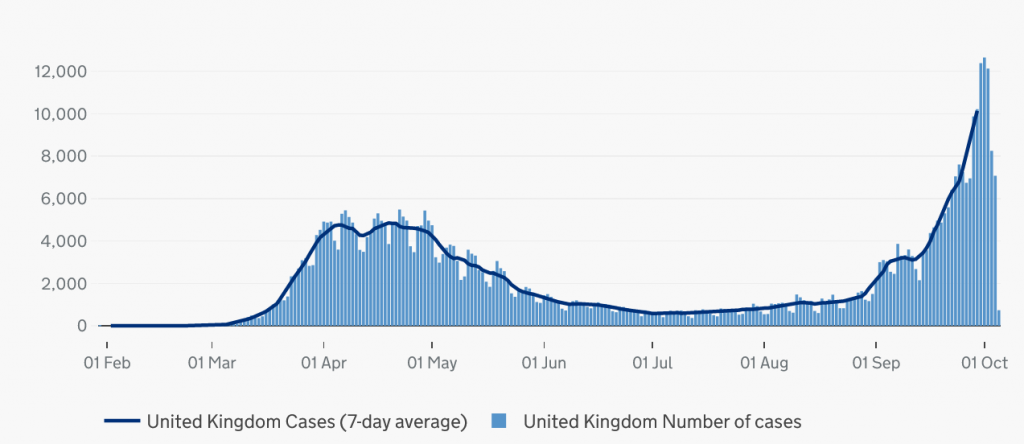
The focus of almost all current reporting on COVID-19 is on the sharp increase in number of ‘new cases’ – as shown in the above graph – and the accompanying narrative that we are in the midst of an exponential ‘second wave’ increase. For example, there were 12,000 ‘new cases’ on October 2nd compared to just 3,000 on September 2nd – a four-fold increase in four weeks, and more than double the new cases per day now than we had at the peak of the pandemic in March.
This looks frightening. But the massive increase in ‘new cases’ is almost completely explained by factors that have nothing to do with an increasing population health risk. New cases are simply the count of those who get a positive test result. But almost all of those – as can be seen from the university student ‘cases’ – are either asymptomatic or false positives., i.e. they do not – and will not – show any symptoms of a ‘COVID-19 illness’. Nor will they ‘spread the virus’ to others.
Also, contrary to widely believed assumptions, there is no ‘gold standard’ test for COVID-19. A diagnostic process, namely PCR, has been used, but since the outbreak there has been no attempt to determine its accuracy. It might be shocking to find that research on lab grown ‘live’ cultures of the virus, taken from patients, had not been published until early August – eight months after the virus outbreak. These have been used to assess the accuracy of PCR and the results are not good. It has been shown it is possible to return a positive PCR test where a sample taken from the same patient never grows a viral culture – meaning the patient does not have an active COVID-19 infection despite the positive PCR test. The implications of this for the false positive rate of PCR tests are obvious and significant.
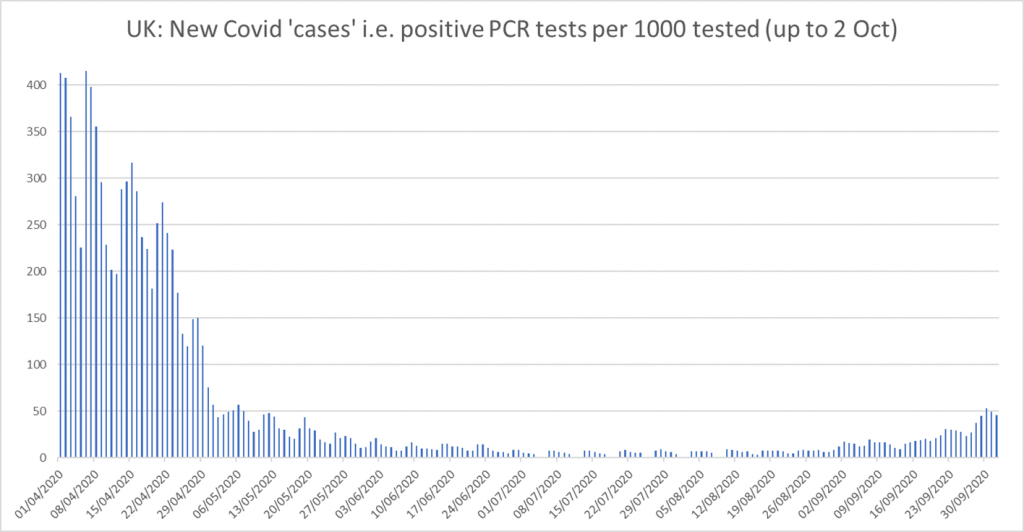
The other obvious explanation for the increase in number of ‘cases’ is that far more people are being tested – 280,000 per day now compared to 10,000 at the peak in March. So, while there are twice the number of ‘new cases’ per day now compared to the March peak, the number of ‘new cases’ per 1000 people tested now is actually only ONE-TENTH of that in the March peak (45 compared to 450). See graph below.
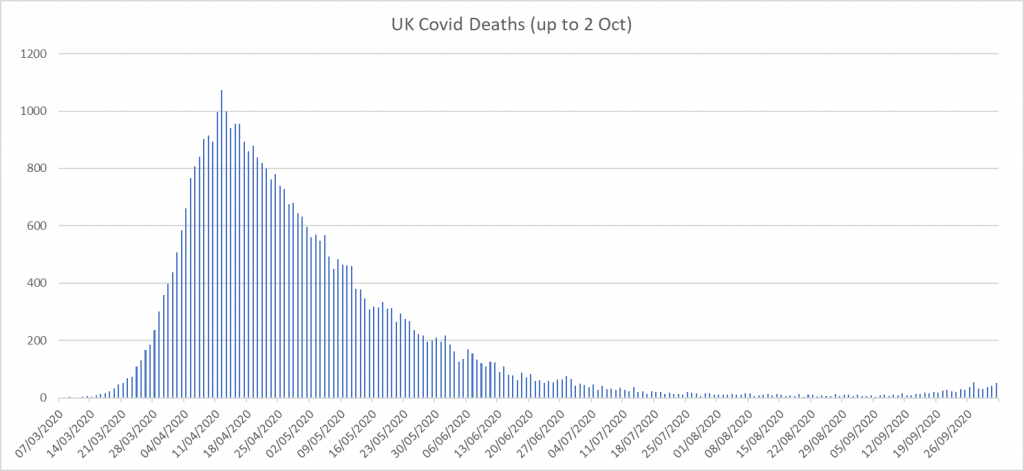
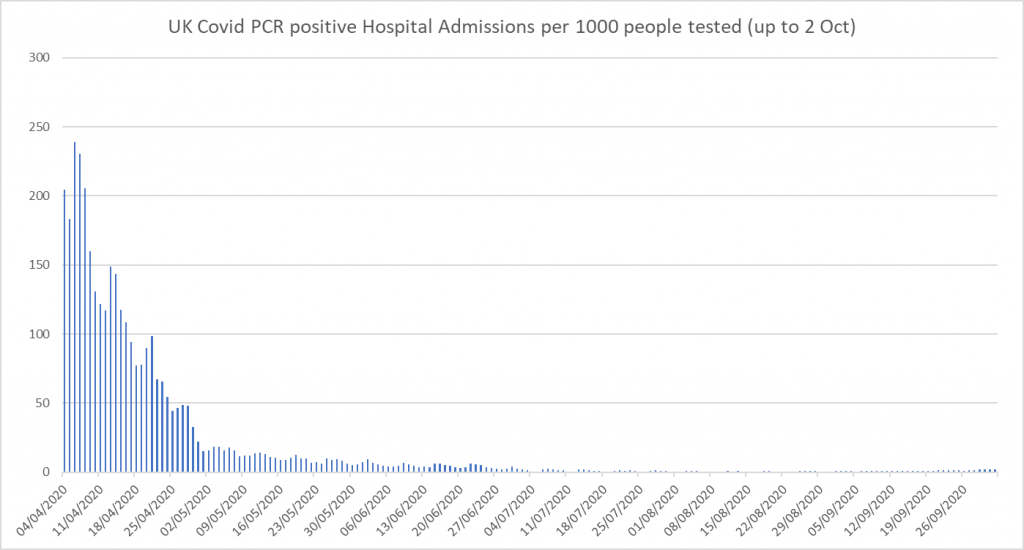
Much of this is borne out by simply looking at the more important trend of “COVID-19” hospital admissions and deaths (see graph below). For both we see increases – but at much slower rates than ‘cases’, and not beyond what we would expect at the beginning of any flu season. But, critically, these counts of ‘COVID-19’ admissions and deaths are inevitably ALSO inflated for the same reason that ‘cases’ are: anybody admitted to hospital – or dying – with a positive test is classified as ‘COVID-19’ irrespective of the actual reason for admission or cause of death AND regardless of whether they showed any symptoms of a ‘COVID-19 illness’. The analogous situation would be assigning the cause of hospitalisation or death to ’a cold’ if a patient harboured a cold virus without showing any symptoms of it.
Professor Norman Fenton is the Professor of Risk and Information Management, School of Electronic and Electrical Engineering, Queen Mary University of London
Dr. Scott McLachlan is a Postdoctoral Research Assistant, School of Electronic and Electrical Engineering, Queen Mary University of London
Professor Martin Neil is the Professor of Computer Science and Statistics, School of Electronic and Electrical Engineering, Queen Mary University of London
Dr. Magda Osman is a Reader in Experimental Cognitive Psychology, School of Biological and Chemical Sciences, Queen Mary University of London










Donate
We depend on your donations to keep this site going. Please give what you can.
Donate TodayComment on this Article
You’ll need to set up an account to comment if you don’t already have one. We ask for a minimum donation of £5 if you'd like to make a comment or post in our Forums.
Sign UpLatest News
Next PostLatest News